In an era defined by rapid technological advancement and profound political polarization, the American public’s relationship with health information is undergoing a seismic shift. New data from KFF’s comprehensive tracking polls reveals a landscape where traditional authorities—once the bedrock of public health guidance—are increasingly viewed through a lens of skepticism, while personal doctors remain the final bastion of credibility for a fragmented electorate.

The Hierarchy of Trust: Doctors vs. Institutions
At the core of the American health experience remains the individual provider. KFF polling confirms that, regardless of political affiliation, race, or educational background, doctors and other frontline health care providers are the most trusted sources for reliable health information. This reflects a persistent, localized trust in the patient-provider relationship, even as faith in broader systemic structures wanes.
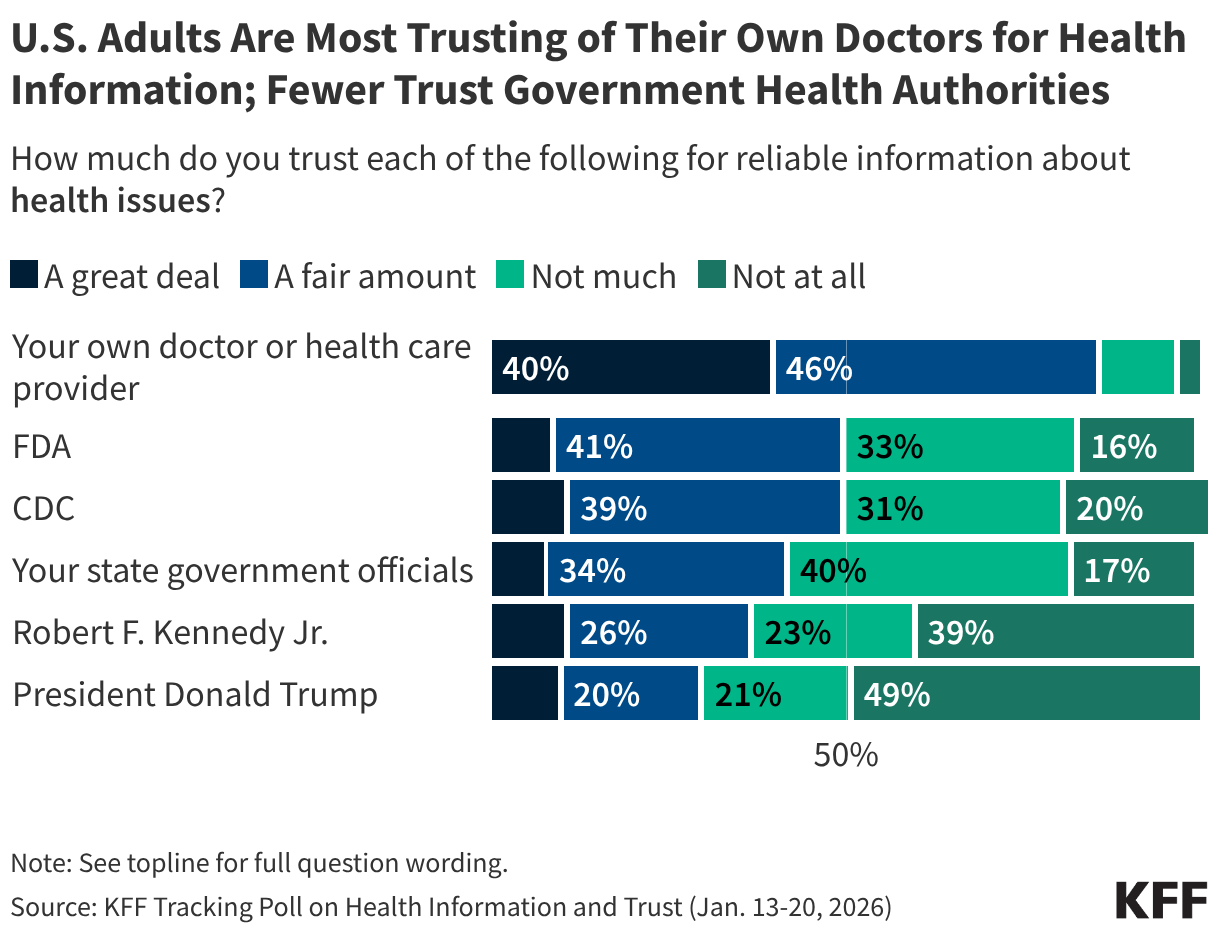
Conversely, trust in government health agencies—the CDC, the FDA, and the Department of Health and Human Services (HHS)—is deeply divided. While a majority of the public still expresses a "fair amount" of trust in their own physicians, only half of adults express similar confidence in the CDC or FDA. This skepticism is even more pronounced regarding specific political figures, including HHS Secretary Robert F. Kennedy Jr. and President Trump, whose reputations as health messengers are bifurcated along sharp partisan lines.
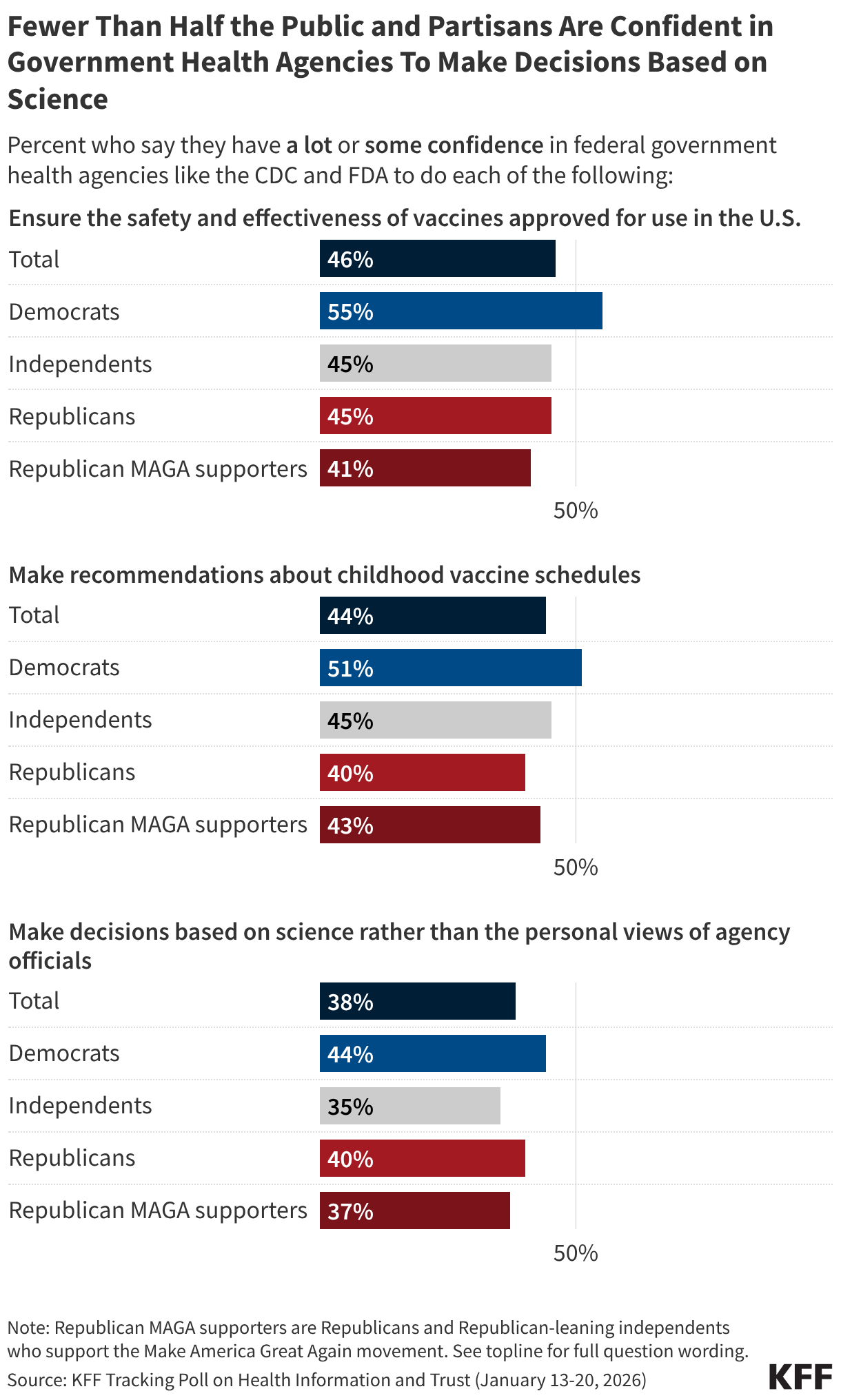
Chronology of Declining Institutional Faith
The degradation of public trust in health agencies did not happen in a vacuum. It is the result of a multi-year trajectory that began with the onset of the COVID-19 pandemic and has since accelerated.
- 2020: The Peak of Bipartisan Cooperation: At the start of the pandemic, the CDC enjoyed broad, bipartisan support as the primary source of truth regarding the emerging virus.
- 2021–2023: The Partisan Wedge: As the pandemic wore on, political narratives around vaccine mandates and public health restrictions began to solidify. Trust in the CDC saw a precipitous drop, particularly among Republicans, fueled by evolving public health guidance and political rhetoric.
- 2025: Political Realignment: The reelection of President Trump and the subsequent appointment of Robert F. Kennedy Jr. as HHS Secretary catalyzed a new shift. While Republican trust in these figures soared—reaching as high as three-quarters among MAGA-aligned voters—Democratic trust in federal health institutions began to wane, reflecting a broader disillusionment with the politicization of science.
- 2026: The New Normal: Today, we see a "malleable middle"—a significant segment of the population that is neither fully convinced of mainstream scientific consensus nor entirely committed to anti-establishment narratives, leaving them vulnerable to misinformation.
Supporting Data: The Anatomy of Skepticism
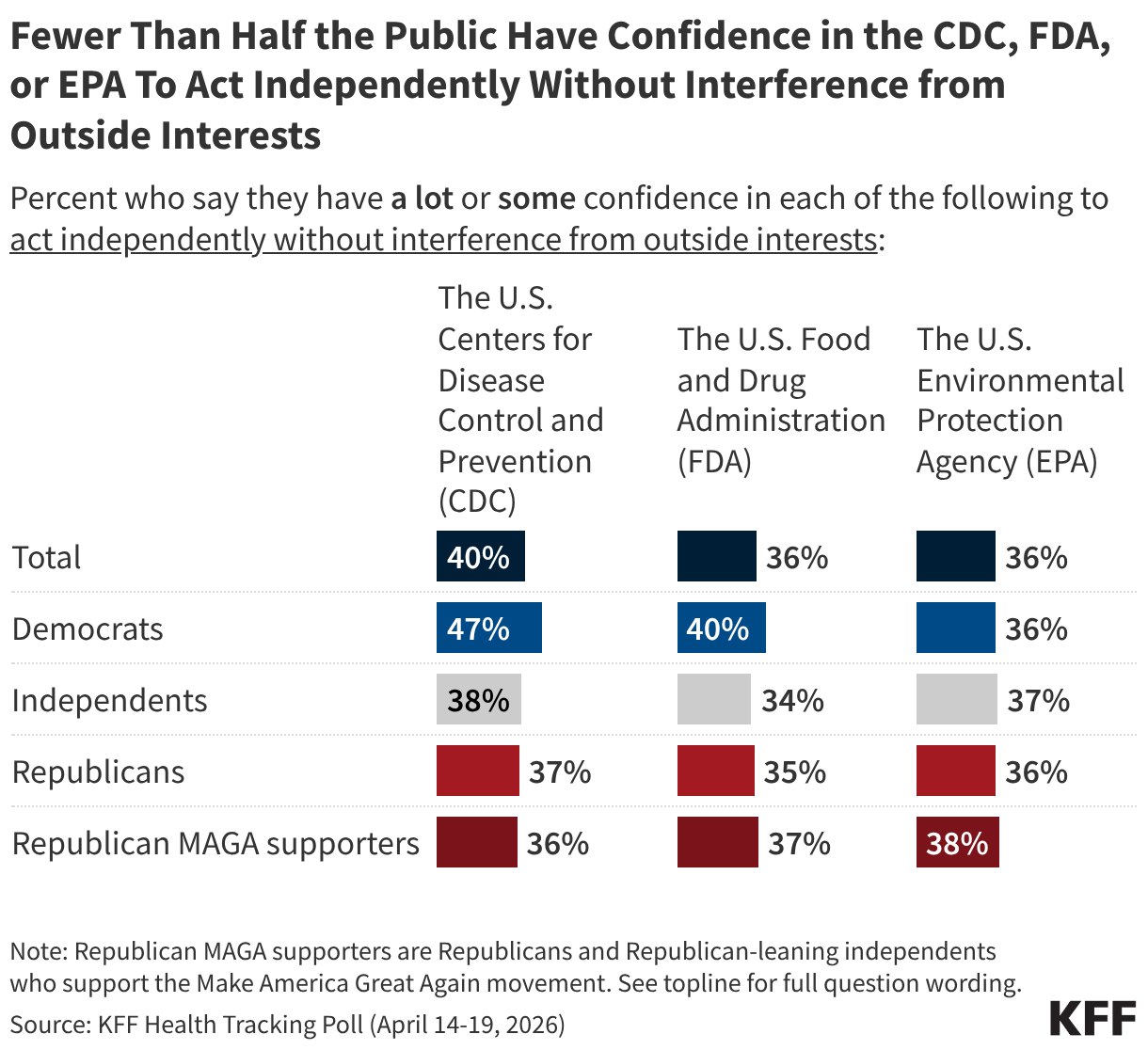
The data paints a stark picture of institutional vulnerability. Fewer than half of U.S. adults believe that agencies like the CDC, FDA, or EPA can act independently without external interference. This perception of "captured" agencies—where political or corporate interests are believed to override scientific rigor—is a major driver of vaccine hesitancy.
The Role of Partisanship
Partisanship is the primary lens through which health information is filtered. While Democrats and Republicans show similar levels of trust in their individual doctors, they diverge sharply on federal authorities. For instance, while both parties show low levels of confidence in the independence of the FDA, Democrats are marginally more likely to trust the CDC. Meanwhile, Republican support for Secretary Kennedy and President Trump acts as a powerful signal, creating an alternative "information ecosystem" that operates independently of traditional medical consensus.
The "Malleable Middle"
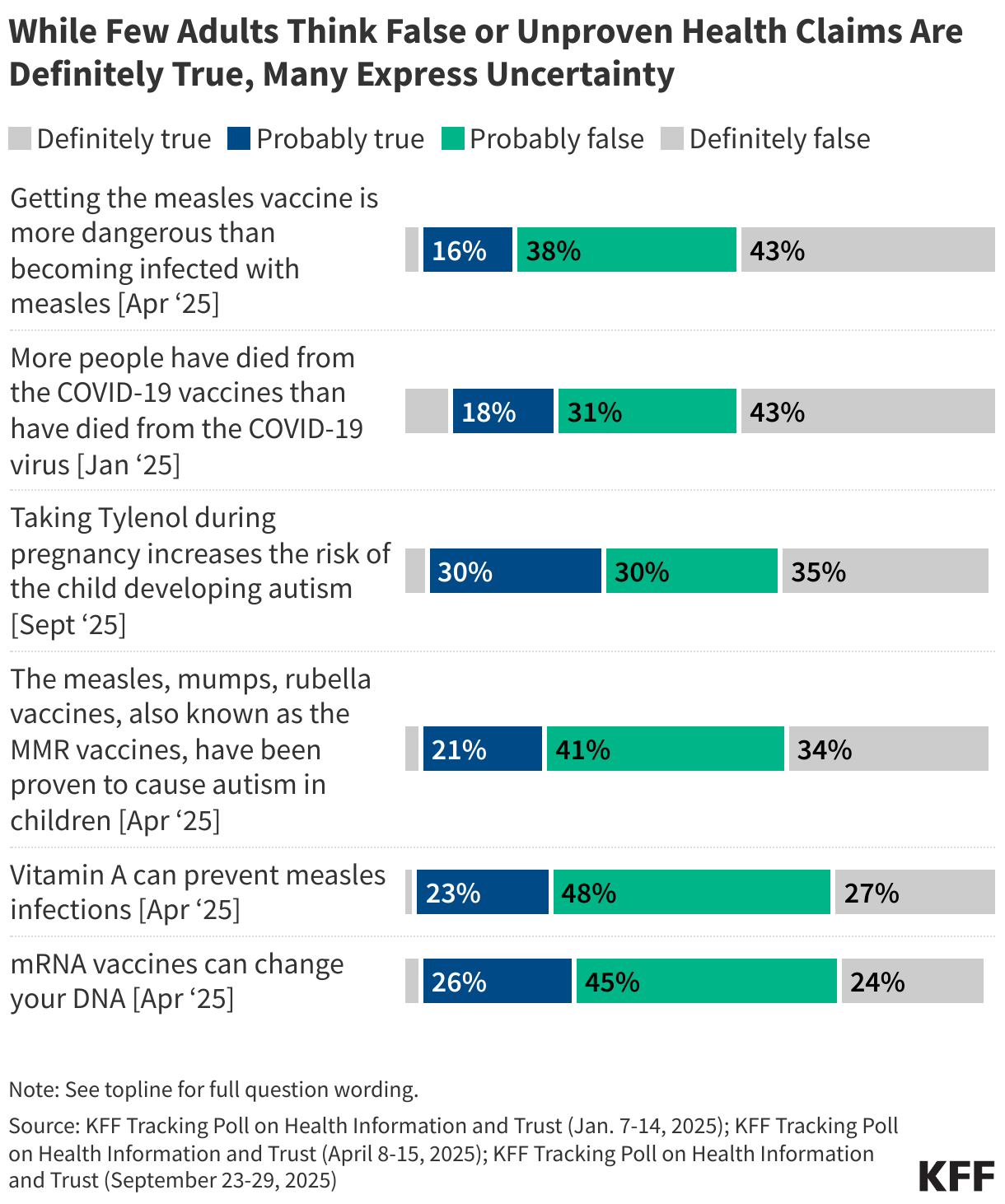
KFF’s research into health misinformation reveals that while only a small minority of Americans are "true believers" in fringe health claims, a vast "malleable middle" exists. Many Americans are uncertain about the veracity of claims—such as a purported link between Tylenol and autism or the safety of childhood vaccine schedules. This uncertainty is not necessarily a product of malice, but of the overwhelming volume of contradictory information available online, which makes it increasingly difficult for the average citizen to distinguish between peer-reviewed science and anecdotal conjecture.
The Digital Frontier: Social Media and AI
As traditional media’s influence wanes, the public is turning to newer, less regulated channels for health advice.
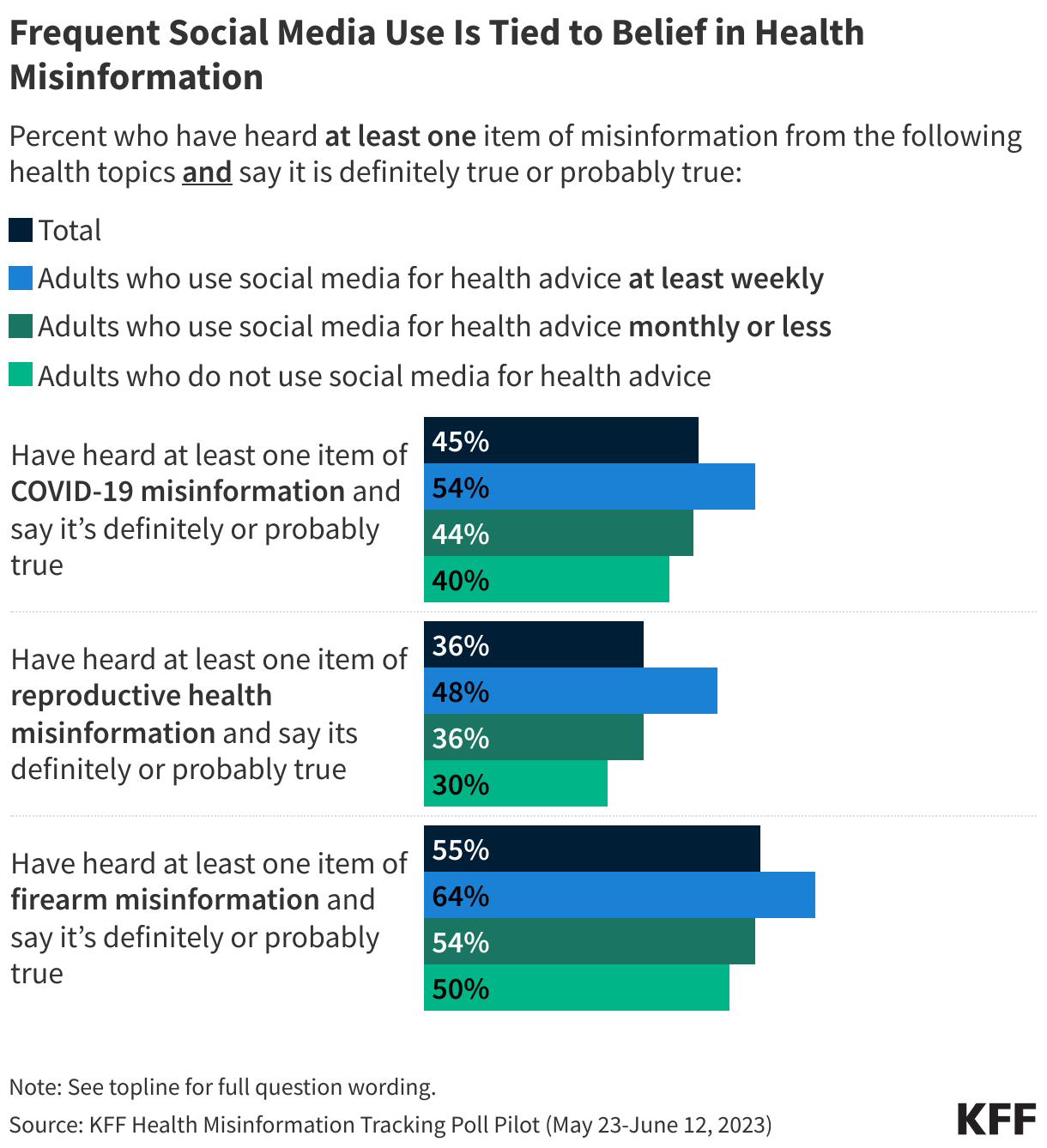
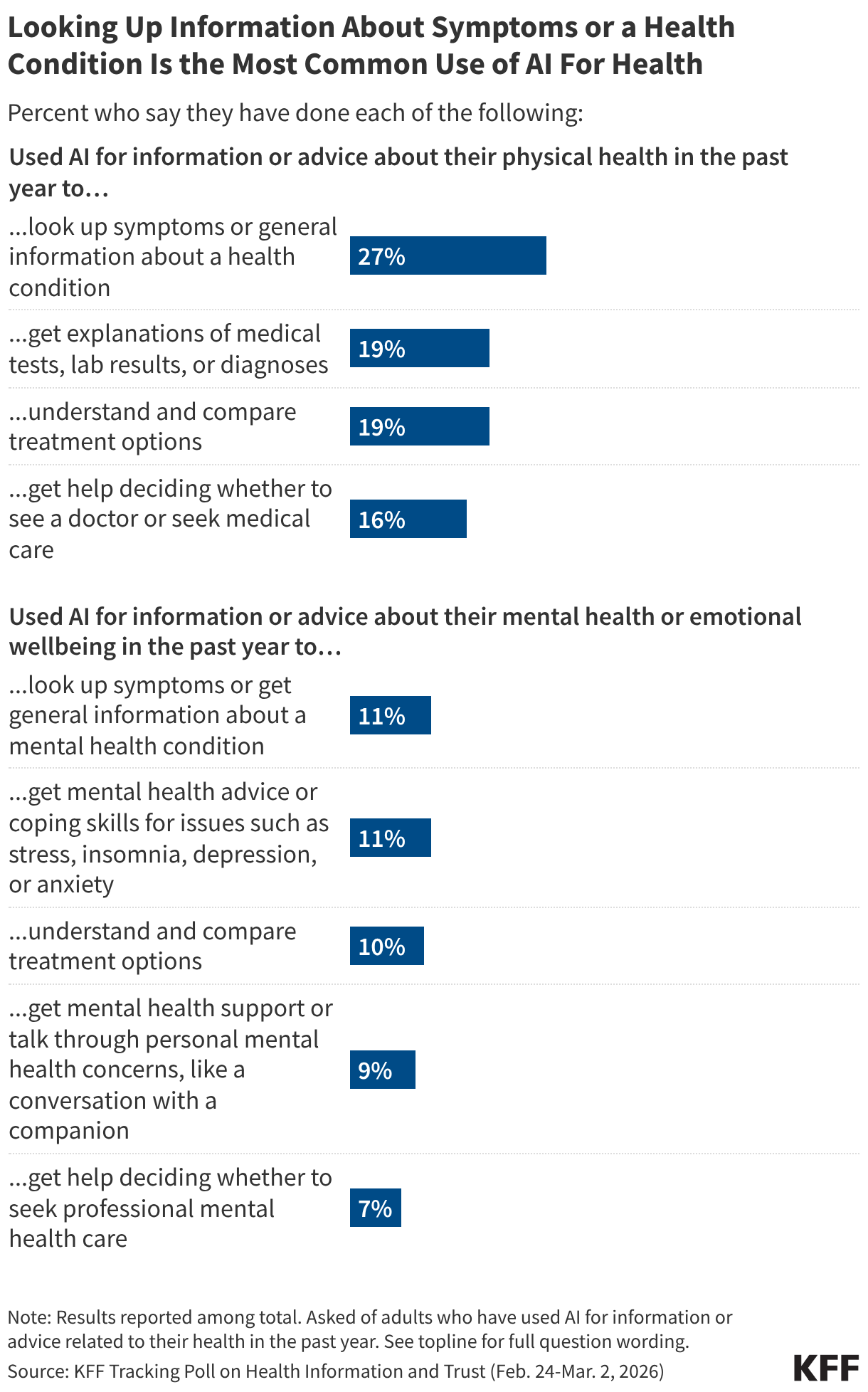
The Rise of AI Chatbots
Nearly one-third of the American public has turned to AI chatbots for health information in the past year. This represents a significant shift in how people perform "triage" for their symptoms. While most users are turning to AI for convenience and speed, a notable percentage of the uninsured and those with limited access to care view AI as a substitute for professional consultation. While the public generally reports low trust in AI, those who use it regularly often report high levels of confidence in the specific advice they receive, highlighting a dangerous "echo chamber" effect.
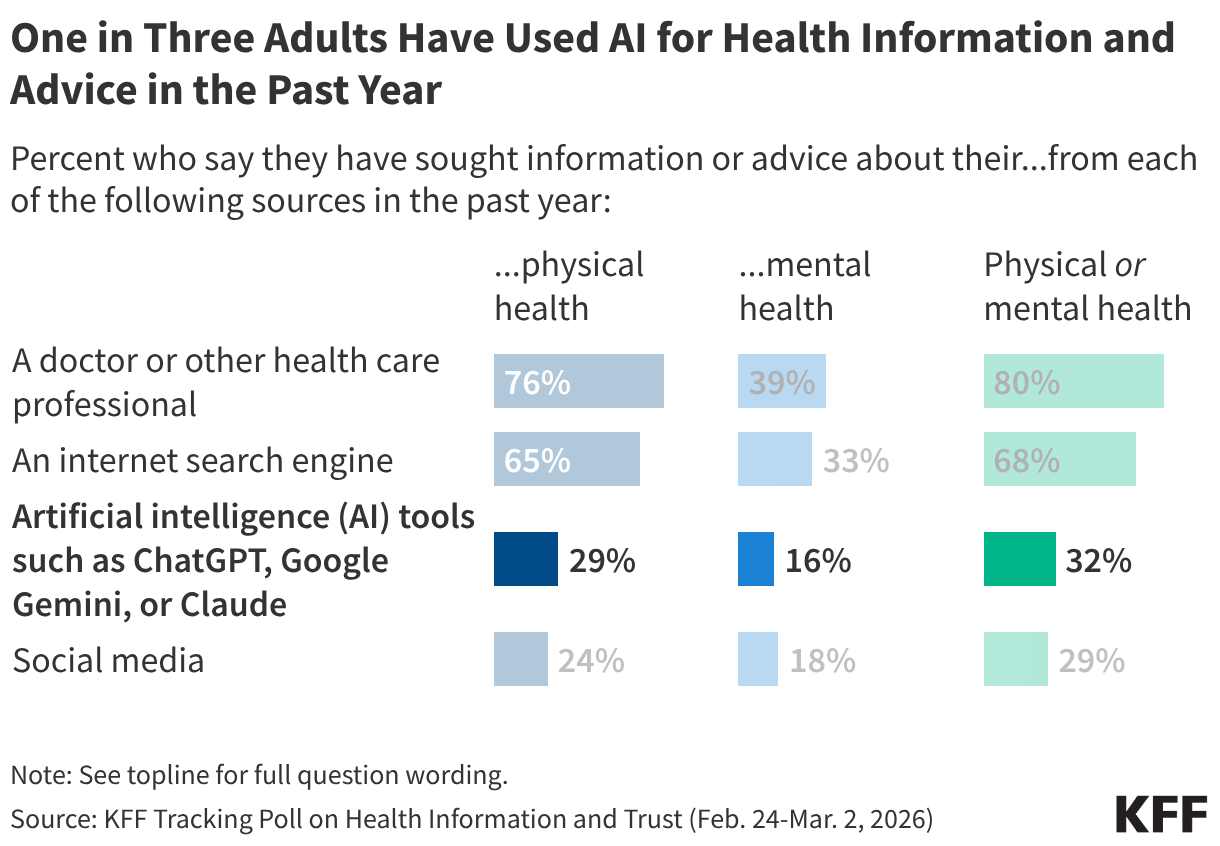
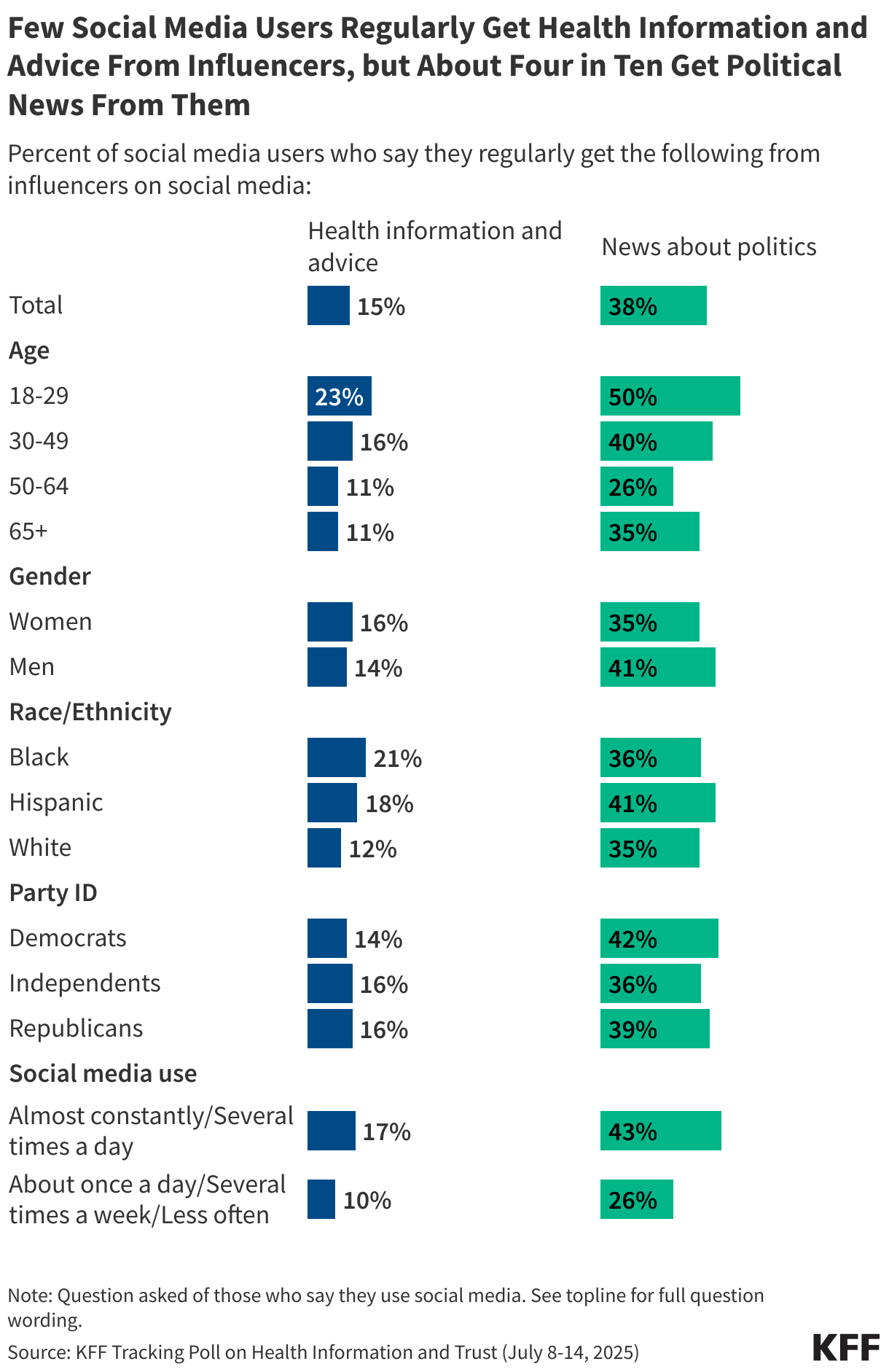
The Influencer Economy
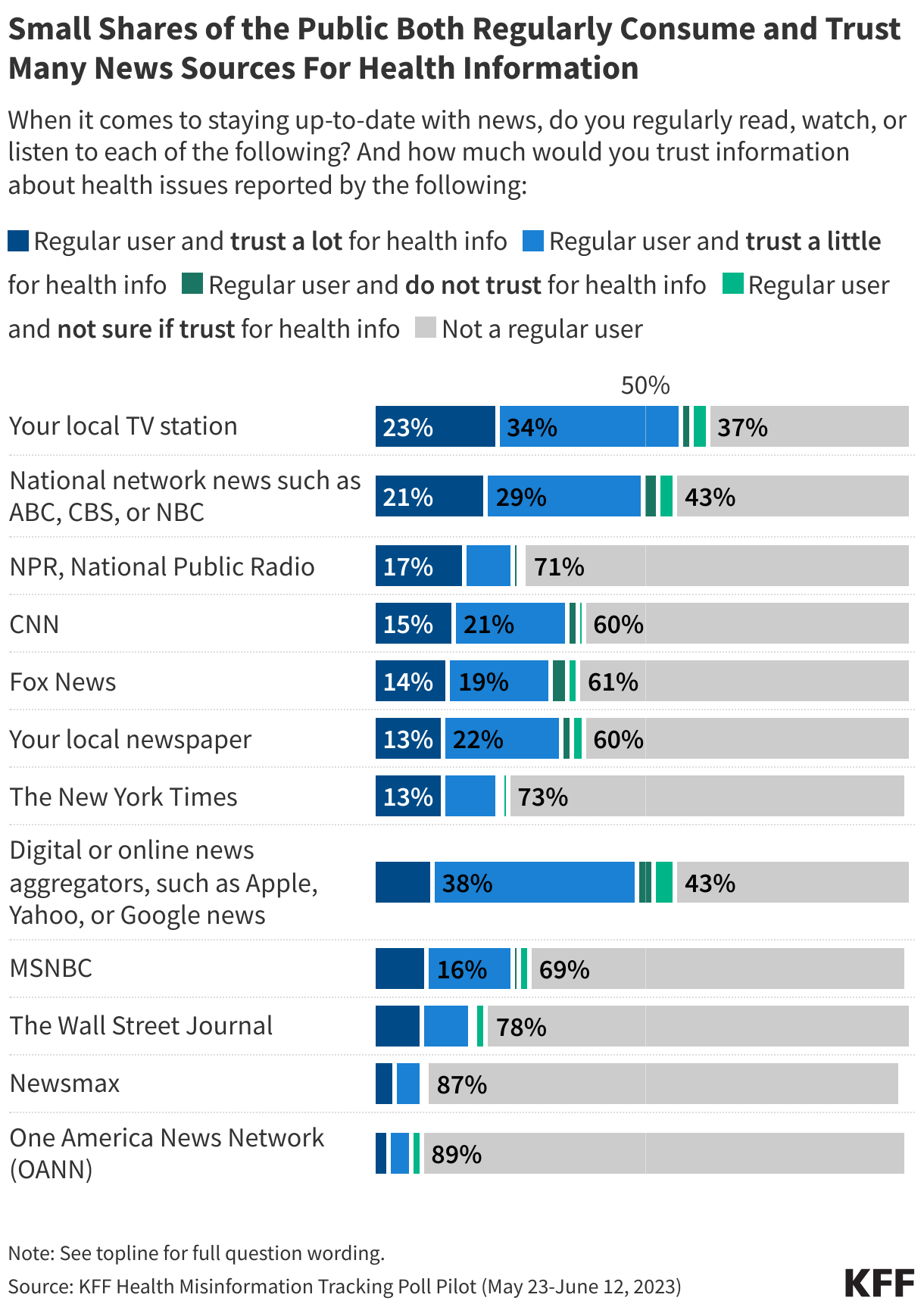
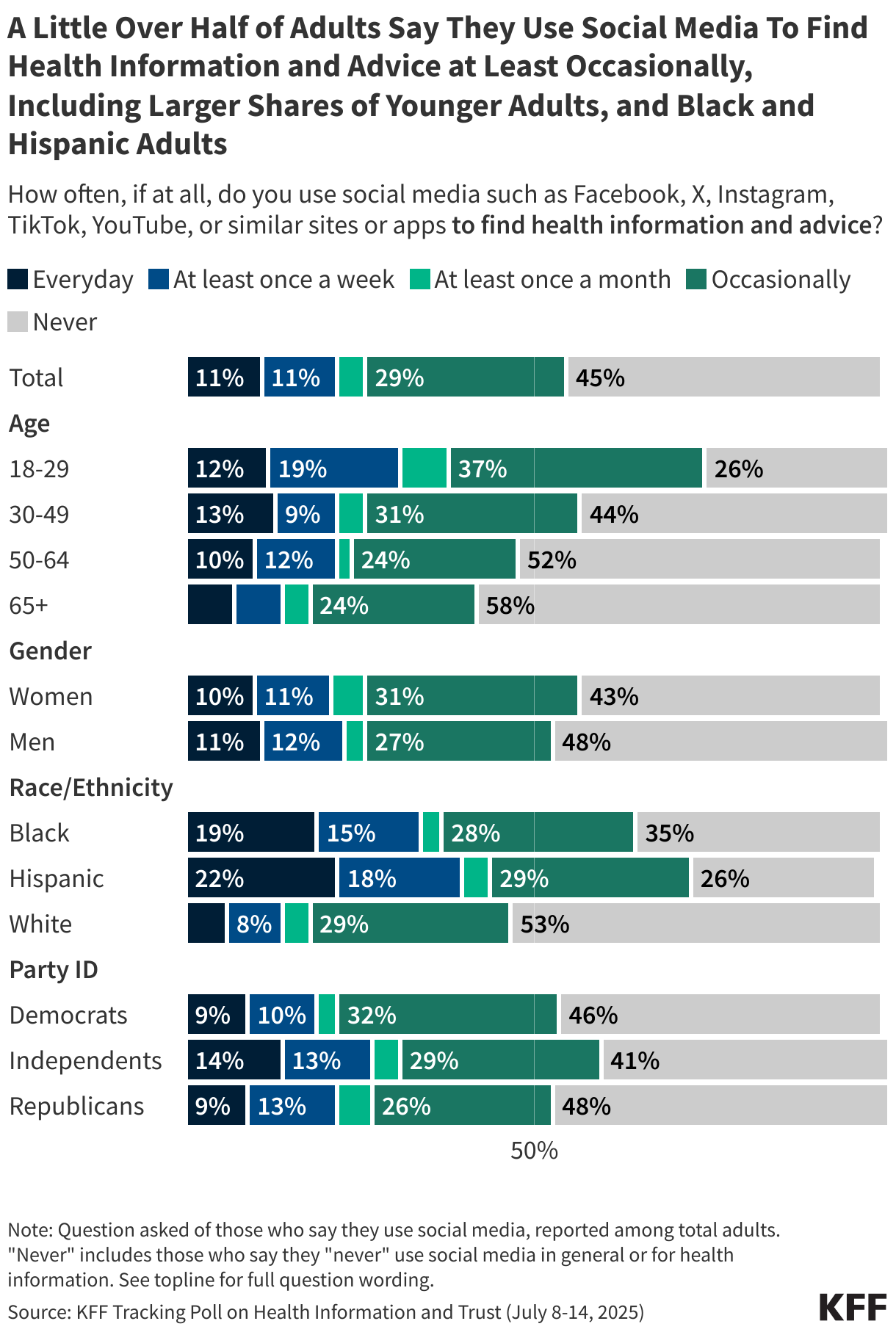
While social media is a primary source of health information, particularly for younger adults and minority communities, it is also a vector for misinformation. The data suggests that frequent social media users are more susceptible to believing false claims regarding reproductive health, firearms, and vaccine safety. Though influencers currently play a smaller role in health advice than they do in political news, their reach is growing, particularly among younger demographics who are increasingly alienated from legacy institutions.
Implications: The Future of Public Health
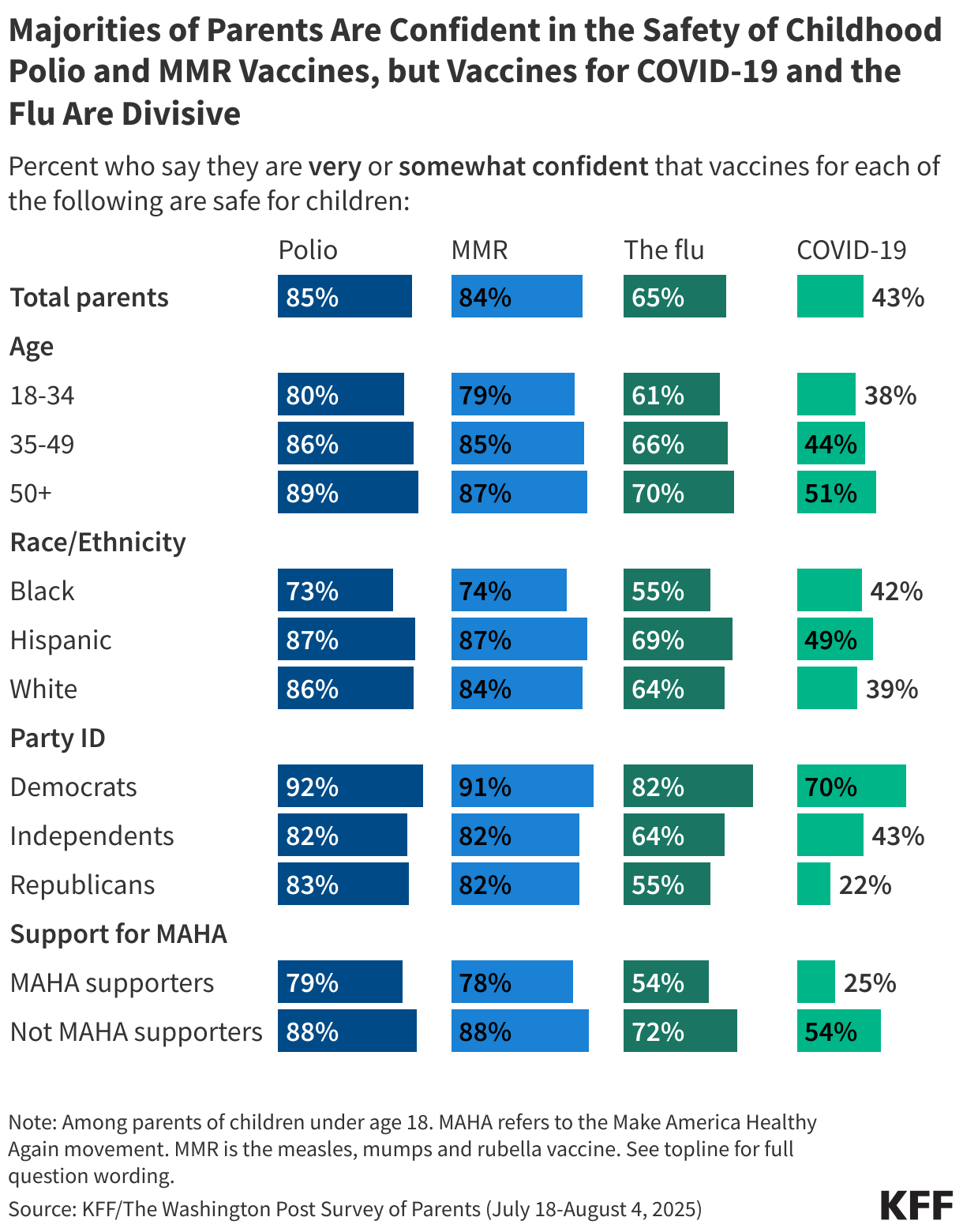
The erosion of trust has tangible consequences. When parents skip or delay routine vaccinations—a behavior now observed in approximately one in six households—the entire public health infrastructure faces increased risk.
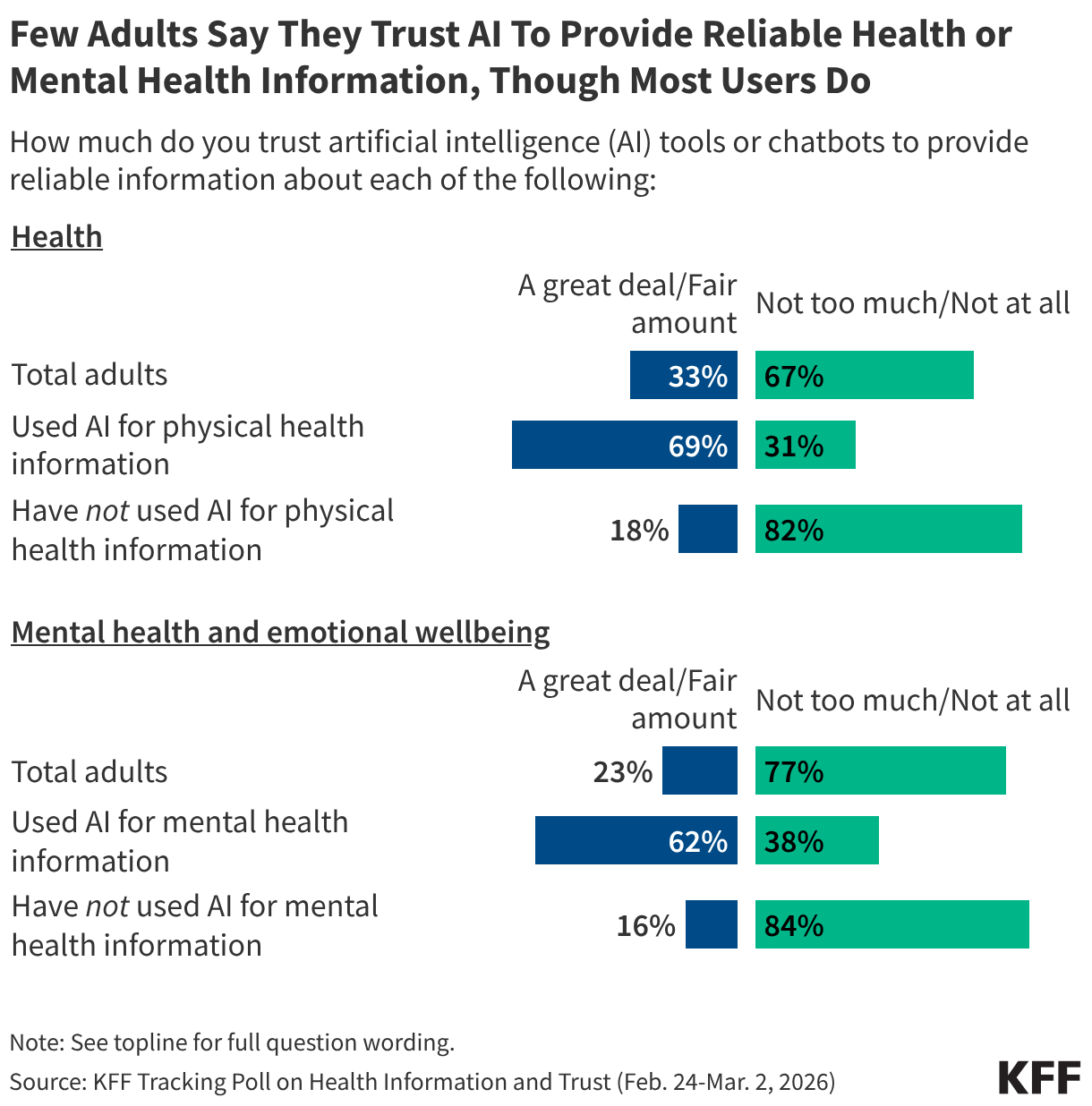
The Challenge of Communication
The primary challenge for public health officials is no longer just the dissemination of information, but the re-establishment of authority. The KFF data suggests that top-down communication from federal agencies is increasingly ineffective, and in some cases, counterproductive. Future interventions may need to be more localized, relying on trusted community messengers—such as local pediatricians and primary care physicians—rather than distant federal officials.
Policy Responses
The government faces a delicate balancing act. Attempting to censor misinformation or aggressively countering it can often trigger a "backfire effect," where distrusting groups become more entrenched in their beliefs. Instead, experts suggest a "pre-bunking" strategy: proactively equipping the public with the tools to identify misinformation before they encounter it, and focusing on the transparency of the scientific process to rebuild the perception of institutional independence.

Conclusion
The current state of health information in America is defined by a paradox: we have unprecedented access to the world’s medical knowledge, yet we have never been more confused about what is true. The shift away from centralized, trusted authorities toward a fractured, personality-driven, and AI-assisted information environment is not merely a trend—it is a transformation of the social contract.
Rebuilding trust will require more than just better fact-checking. It will require a fundamental rethink of how health information is delivered, who delivers it, and how we address the underlying systemic anxieties—ranging from health care costs to political alienation—that drive the American public away from established science and toward the allure of the alternative. As we look toward the remainder of the decade, the ability of our institutions to adapt to this new reality will likely determine the trajectory of the nation’s public health outcomes for generations to come.