LOS ANGELES, CA – [Date] – In a significant development poised to redefine the battle against glioblastoma, a highly aggressive and notoriously lethal form of brain cancer, a new study led by researchers at Keck Medicine of USC has unveiled a promising combination therapy. The findings suggest that integrating Tumor Treating Fields (TTFields) therapy with both immunotherapy (pembrolizumab) and conventional chemotherapy (temozolomide) could dramatically extend survival rates for patients, including those with previously inoperable tumors. This breakthrough offers a beacon of hope in a medical landscape where effective treatments for glioblastoma have remained tragically scarce.
According to the National Brain Tumor Society, the average survival for patients diagnosed with glioblastoma stands at a grim eight months, highlighting the urgent need for innovative therapeutic strategies. This new research, spearheaded by Dr. David Tran, Chief of Neuro-Oncology with Keck Medicine and co-director of the USC Brain Tumor Center, presents a compelling case for a synergistic approach that primes the body’s immune system to attack the cancer more effectively. The study, building upon years of dedicated research, indicates a potential paradigm shift, transforming previously ineffective immunotherapies into powerful allies against this formidable disease.
Understanding Glioblastoma: A Formidable Foe
Glioblastoma multiforme (GBM) is the most common and aggressive primary brain tumor in adults. Characterized by its rapid growth, highly invasive nature, and resistance to conventional treatments, GBM has long presented one of oncology’s most intractable challenges. Despite advancements in surgical techniques, radiation therapy, and chemotherapy, patient prognosis remains severely limited. The tumor’s location within the brain, protected by the formidable blood-brain barrier, and its inherent ability to create an immunosuppressive microenvironment, contribute significantly to its resistance to many systemic therapies, including those that have shown remarkable success in other cancer types.
The standard of care for newly diagnosed glioblastoma typically involves maximal safe surgical resection, followed by concurrent radiation therapy and temozolomide chemotherapy. While this regimen can offer a temporary reprieve, recurrence is almost inevitable, and subsequent treatment options are often palliative, focusing on symptom management rather than curative intent. The dire statistics underscore a critical unmet need for therapies that can not only extend life but also improve the quality of life for those afflicted by this devastating diagnosis.
The Dawn of a New Hope: A Synergistic Approach
The Keck Medicine of USC study, analyzing data from the 2-THE-TOP Phase 2 clinical trial, posits that the strategic combination of TTFields therapy, immunotherapy with pembrolizumab, and temozolomide chemotherapy creates a powerful multi-pronged attack against glioblastoma. This tripartite regimen demonstrated a remarkable association with a 70% increase in overall survival compared to historical data, a statistic that resonates profoundly within the neuro-oncology community.
"Our findings suggest that TTFields may be the key to unlocking the value of immunotherapy in treating glioblastoma," stated Dr. Tran, who is also a corresponding author of the study. He further elaborated, "By using TTFields with immunotherapy, we prime the body to mount an attack on the cancer, which enables the immunotherapy to have a meaningful effect in ways that it could not before." This statement encapsulates the core premise of the research: transforming an environment traditionally hostile to immune intervention into one receptive to it.
Unpacking the Therapeutic Arsenal: Mechanisms of Action
To fully appreciate the significance of this combination, it’s crucial to understand the individual components and how they interact synergistically.
Tumor Treating Fields (TTFields): Disrupting Cellular Division
TTFields therapy, delivered by a device known as Optune (manufactured by Novocure), represents a unique non-invasive anti-mitotic treatment. It works by delivering low-intensity, alternating electric fields directly into tumors. These targeted electric waves exert physical forces on key intracellular structures during cell division, specifically disrupting the formation of the mitotic spindle, which is essential for cell proliferation. By continuously pushing and pulling these structures in shifting directions, TTFields make it difficult for cancer cells to multiply, effectively halting tumor growth and leading to cell death.
For glioblastoma patients, TTFields are delivered via a set of mesh electrodes strategically positioned on the scalp, generating fields at a precise frequency and intensity focused on the tumor. Patients typically wear these electrodes for approximately 18 hours a day, a commitment that underscores the intensity of the treatment, yet offers a life-extending benefit. Beyond its direct anti-proliferative effects, the study further reveals that TTFields play a crucial role in immune modulation, attracting more tumor-fighting T cells—a type of white blood cell vital for identifying and attacking cancer cells—into and around the glioblastoma. This critical recruitment sets the stage for immunotherapy.
Immunotherapy’s Elusive Promise: Unleashing the Body’s Defenders
Pembrolizumab, the immunotherapy agent used in this study, is an immune checkpoint inhibitor (ICI). ICIs work by blocking specific proteins (checkpoints) on immune cells, such as PD-1, that normally prevent T cells from attacking healthy cells. By inhibiting these checkpoints, pembrolizumab essentially "removes the brakes" from the immune system, allowing T cells to more effectively recognize and destroy cancer cells. This approach has revolutionized the treatment of many cancers, including melanoma, lung cancer, and kidney cancer.
However, immunotherapy has historically struggled against glioblastoma. The primary reason for this failure lies in the brain’s unique anatomy and physiology. The blood-brain barrier (BBB), a highly selective semipermeable border of endothelial cells, protects the brain from circulating toxins and pathogens but also restricts the entry of many therapeutic agents and, crucially, immune cells like T cells. Consequently, glioblastomas are characterized by an immunosuppressive "cold" microenvironment, meaning there are very few T cells in and around the tumor to begin with. Without a robust initial immune presence, ICIs like pembrolizumab have little to amplify, rendering them largely ineffective when used alone for glioblastoma.
Temozolomide: The Chemotherapeutic Foundation
Temozolomide (TMZ) is an oral alkylating agent that has been the cornerstone of glioblastoma chemotherapy since its approval. It works by damaging the DNA of cancer cells, leading to their death. While effective in some patients, particularly those with a methylated MGMT gene promoter (a biomarker indicating better response to TMZ), its efficacy is often limited by tumor resistance and the overall aggressive nature of glioblastoma. In the context of this new combination, TMZ serves as a foundational chemotherapy, contributing to tumor burden reduction and potentially enhancing the immune response through immunogenic cell death.
The Keck Medicine Breakthrough: In Situ Immunization
Dr. Tran’s innovative hypothesis centered on overcoming the glioblastoma’s inherent immunosuppression not by trying to breach the blood-brain barrier from the outside, but by initiating an immune reaction directly within the tumor itself—an approach known as "in situ immunization." He theorized that TTFields, with their direct physical impact on tumor cells, could serve as the crucial trigger for this localized immune activation.
The study’s observations strongly support this theory. Researchers found that TTFields not only disrupt tumor growth but also actively attract more tumor-fighting T cells into and around the glioblastoma. This influx of T cells, critical for an effective immune response, fundamentally changes the tumor microenvironment from "cold" to "hot." Once these T cells are present, the subsequent administration of immunotherapy (pembrolizumab) becomes profoundly more effective. Pembrolizumab then amplifies the activity of these newly recruited T cells, ensuring they stay active longer and are replaced by even stronger, more effective tumor-fighting T cells.
"Think of it like a team sport – immunotherapy sends players in to attack the tumor (the offense), while TTFields weaken the tumor’s ability to fight back (the defense). And just like in team sports, the best defense is a good offense," Dr. Tran eloquently explained, emphasizing the synergistic interplay between the therapies.
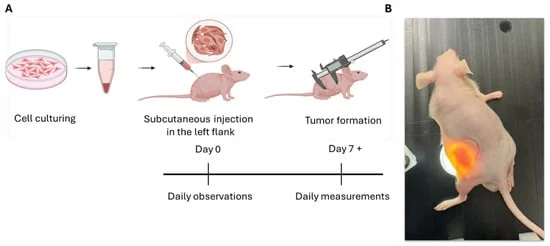
Phase 2 Trial Unveils Remarkable Gains: The 2-THE-TOP Study
The foundation of these promising findings stems from the 2-THE-TOP, a Phase 2 clinical trial. The trial enrolled 31 newly diagnosed glioblastoma patients who had completed initial chemoradiation therapy. Of this cohort, 26 patients received the novel triple combination of TTFields, chemotherapy (temozolomide), and immunotherapy (pembrolizumab).
The treatment protocol involved patients receiving six to twelve monthly treatments of chemotherapy alongside TTFields for up to 24 months, with duration determined by individual patient response. Immunotherapy was administered every three weeks, starting with the second dose of chemotherapy, for up to 24 months.
The results were compelling:
- Significantly Extended Survival: Patients who received the combination therapy lived approximately 10 months longer than historical control patients who had used TTFields with chemotherapy alone in the past. This represents a substantial improvement in a disease where every month gained is precious.
- Unprecedented Response in Unresected Tumors: Perhaps one of the most remarkable findings was the exceptional response observed in patients with larger, unresected (not surgically removed) tumors. Seven of the 26 patients in the combination therapy arm had inoperable tumors due to their challenging locations – a subgroup with the worst prognosis and severely limited treatment options. These patients, against all odds, lived approximately 13 months longer than their resected counterparts and demonstrated a much stronger immune activation. This counter-intuitive result suggests that, in the context of kick-starting the body’s immune response, a larger tumor may actually provide more targets for the TTFields to activate and for the immune system to subsequently attack.
- Enhanced Immune Activation: The study provided clear evidence that the combination therapy successfully triggered a potent immune response within the tumor, which was then amplified by the immune checkpoint inhibitor.
"Further studies are needed to determine the optimal role of surgery in this setting, but these findings may offer hope, particularly for glioblastoma patients who do not have surgery as an option," Dr. Tran noted, highlighting the profound implications for a previously underserved patient population.
Expert Perspectives: Unlocking Immunotherapy’s Potential
The consensus among the research team is that this combination therapy fundamentally alters the tumor microenvironment, making glioblastoma susceptible to immunotherapeutic strategies that were previously ineffective. Dr. Tran, with over a decade of research into TTFields, believes these findings are not merely incremental but represent a potential paradigm shift.
"Immunotherapy has been a game-changer for many cancers, but glioblastoma has remained stubbornly resistant. We’ve always believed in the potential of the immune system to fight brain tumors, but the challenge was how to bypass the unique protective mechanisms of the brain," Dr. Tran elaborated. "This study provides a roadmap. TTFields don’t just kill tumor cells; they make them visible and vulnerable to the very immune cells that were previously locked out or ineffective."
The research also sheds light on the intricacies of the tumor’s defense mechanisms. By understanding how TTFields can overcome the immunosuppressive environment, future research can further refine these strategies, potentially leading to even more potent combinations or targeted therapies.
Beyond the Horizon: The Crucial Phase 3 Validation
While the Phase 2 results are highly encouraging, the medical community emphasizes the critical need for validation in a larger, multicenter Phase 3 clinical trial. Keck Medicine of USC is at the forefront of this crucial next step, actively participating in the global Phase 3 trial designed to definitively assess the efficacy of TTFields in combination with immunotherapy and chemotherapy.
Dr. Tran, recognizing the importance of this validation, serves as the chair of the steering committee for this expansive trial. Dr. Frances Chow, a neuro-oncologist with USC Norris, is the principal investigator of the Keck Medicine study site, ensuring local expertise contributes to the global effort.
This ambitious Phase 3 trial, currently open at 28 sites across the United States, Europe, and Israel, aims to enroll over 740 patients through April 2029. The trial is meticulously designed to include patients with various surgical statuses – gross total resection, partial resection, or biopsy-only tumors – to comprehensively assess how the extent of tumor removal influences immune response and overall treatment efficacy. The data from this trial will be instrumental in establishing this combination therapy as a new standard of care, potentially bringing widespread relief and extended life to countless glioblastoma patients worldwide.
A Collaborative Endeavor and Disclosures
This groundbreaking study is the product of extensive collaboration and dedicated effort. Keck School of Medicine of USC authors contributing to this work include Dongjiang Chen, PhD, assistant professor of research neurological surgery; Son Le, PhD, assistant professor of research neurological surgery; Harshit Manektalia, research programmer; Ming Li, PhD, professor of research population and public health sciences; and Adam O’Dell, research lab specialist. Collaborators from the University of Florida, Ashley Ghiaseddin, MD, and Maryam Rahman, MD, MS, also played a vital role in this research.
The study received funding support from Novocure, the manufacturer of Optune, the TTFields device utilized in the research. In the interest of full transparency, Dr. David Tran has disclosed receiving honoraria from Novocure for consultant work. Furthermore, Dr. Chen and Dr. Tran are inventors of two patent applications related to the work reported in this study, underscoring their innovative contributions to the field.
Conclusion
The findings from Keck Medicine of USC represent a monumental stride forward in the relentless fight against glioblastoma. By demonstrating the power of combining Tumor Treating Fields with immunotherapy and chemotherapy, researchers have illuminated a viable path towards significantly extending the lives of patients facing this devastating diagnosis, particularly those for whom surgical options are limited. As the global Phase 3 trial progresses, the scientific community and patient advocates alike await with cautious optimism, hopeful that this synergistic approach will soon translate into a new era of effective glioblastoma treatment, offering not just extended survival, but a renewed sense of hope.