In the high-stakes environment of oncology, the difference between a successful treatment plan and a missed opportunity often comes down to the quality of data. For patients diagnosed with non-small cell lung carcinoma (NSCLC), the precision of staging—determining whether the cancer has spread to the lymph nodes—is the cornerstone of their survival prognosis. A landmark multicentre study published in the journal Cancers (May 2026) has revealed that a simple, structural change in how doctors document procedures is significantly improving patient care across five Australian hospitals.
The research, led by Dr. Ashleigh Witt and a team of respiratory experts, demonstrates that replacing traditional, narrative-based "free-text" reporting with "synoptic reporting"—a standardized, checklist-driven format—substantially improves the quality of Endobronchial Ultrasound (EBUS) procedures.
The Core Problem: The Perils of Free-Text Reporting
Endobronchial ultrasound (EBUS) is the gold-standard procedure for staging the mediastinum (the central compartment of the chest) in lung cancer patients. However, for years, the medical community has grappled with a persistent issue: the variability of procedural documentation.
Traditionally, clinicians have relied on narrative reports—essentially written accounts of the procedure. Because these reports are often unstructured, critical data points are frequently omitted. If a doctor fails to record the status of specific lymph node stations, it creates a "blind spot" in the patient’s medical record. As Dr. Witt and her team noted, this lack of standardization makes it nearly impossible to audit care quality or ensure that patients receive the most appropriate, evidence-based management.
"Procedural documentation is often variable and incomplete due to reliance on free-text reporting," the study authors noted. "Synoptic reporting, which is a structured, standardized approach, ensures consistent documentation of all clinically relevant information."
Chronology: From Concept to Clinical Transformation
The study, titled "Synoptic Reporting Improves Quality of Endobronchial Ultrasound (EBUS): An Australian Multicentre Study," employed an ambispective design to measure the impact of the intervention. The project unfolded across five major metropolitan hospitals in Melbourne, Australia.
- Pre-Intervention Phase (Late 2024): Researchers analyzed three months of historical data, observing the "standard" practice of free-text reporting. During this period, the inconsistencies in documentation were stark.
- The Implementation (November 1, 2024): The research team introduced the synoptic reporting template. At three sites, this was integrated directly into existing reporting software (Endobase or Provation MD), requiring clinicians to fill out mandatory fields before they could finalize a report. At the two remaining sites, the template was provided as a guide for clinicians to use within their existing narrative systems.
- Post-Intervention Phase (Early 2025): The team analyzed the following three months of data to determine if the mandatory structure led to better procedural outcomes.
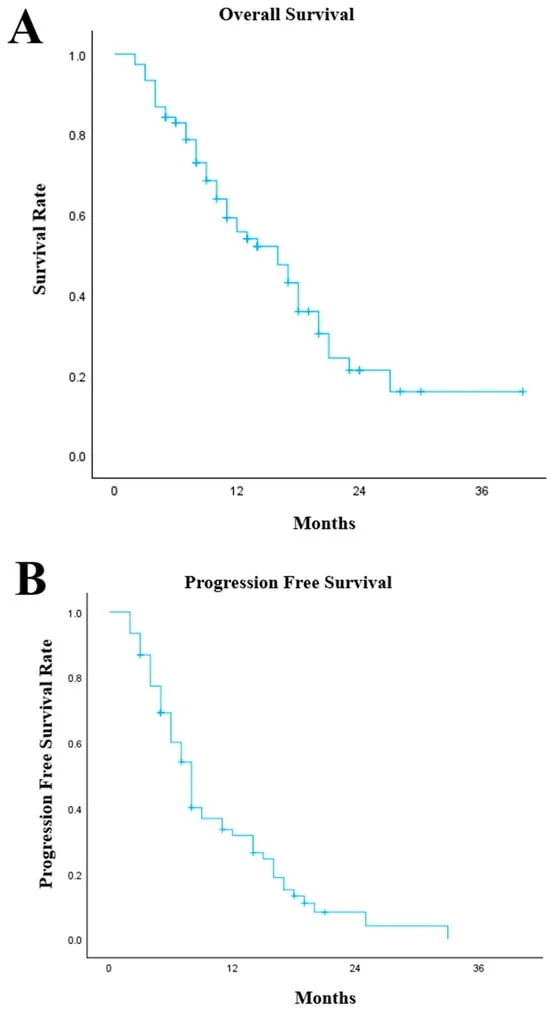
The results were transformative. The study included 96 procedures in the pre-intervention phase and 77 in the post-intervention phase.

Supporting Data: A Measurable Leap in Quality
The data presented by Dr. Witt’s team serves as a compelling argument for the mandatory adoption of synoptic reporting in interventional pulmonology. The findings show significant gains in four key performance areas:
1. Complete Mediastinal Staging
The primary outcome was the "completeness" of the staging—ensuring all five key mediastinal lymph node stations were examined. In the pre-intervention cohort, only 17.7% of procedures met the criteria for complete systematic staging. After the implementation of synoptic reporting, this figure jumped to 87%.
2. Detection of PET-Occult Metastases
One of the most significant clinical findings was the increase in detecting "PET-occult" metastases—cancerous cells in lymph nodes that were not flagged as suspicious on initial PET or CT scans. Before the intervention, only 3.1% of these hidden metastases were detected. With the structured reports, that rate increased to 11.7%. This means that 11.7% of patients were accurately upstaged, allowing them to receive more appropriate, potentially life-saving, non-surgical treatment rather than undergoing a surgery that might have been ineffective or unnecessary.
3. Rigorous Sampling
The study also found that clinicians became more thorough. The mean number of lymph nodes sampled per procedure rose from 1.75 to 2.45. Perhaps more importantly, the rate of sampling radiologically "normal" nodes increased from 38.5% to 71.4%. By forcing the clinician to account for every station, the synoptic report incentivizes a more comprehensive, "leave no stone unturned" approach to the procedure.
4. Reduced Variability
Before the intervention, the rate of complete staging varied wildly between hospitals—ranging from 3.1% to 45.5%. After the intervention, the gap between the best-performing and lowest-performing hospitals narrowed significantly, demonstrating that a standardized system can effectively level the playing field, ensuring that a patient receives the same high quality of care regardless of which facility they visit.
Official Perspectives and Expert Insight
The research highlights a critical distinction: while some hospitals integrated the templates directly into their software (making fields mandatory), others used a non-integrated, "manual" version of the template. Interestingly, both methods saw significant improvements.
"Overall, the effect of the intervention remained highly significant after accounting for clustering by site," the authors stated. This suggests that the intentionality of using a structured format is just as important, if not more so, than the specific software used to host it.

The study also addressed the "Hawthorne Effect"—the idea that doctors might perform better simply because they know they are being observed. While the researchers acknowledged this possibility, they argued that the sustained improvement and the sheer scale of the shift in diagnostic performance suggest that the synoptic format provides a genuine, long-term cognitive aid for practitioners.
Broader Implications: A New Standard for Pulmonology?
The implications of this study reach far beyond the borders of Australia. By providing a scalable, low-cost intervention, Dr. Witt’s team has created a blueprint that could be adopted by respiratory departments worldwide.
Improving Multidisciplinary Teamwork
Cancer care is inherently multidisciplinary. When a surgeon, an oncologist, and a radiologist review a patient’s file, they rely on the EBUS report to make high-stakes decisions. A synoptic report provides these specialists with a clear, reliable, and standardized data set, eliminating the ambiguity often found in long-form narrative notes.
Training the Next Generation
Structured reporting acts as a "guardrail" for less experienced clinicians. By presenting a mandatory checklist of stations to examine, the system serves as an educational tool, guiding trainees through the standard of care and ensuring they do not develop gaps in their procedural technique.
The Path Forward
The research team concludes that while the initial results are promising, the next phase must involve evaluating how these improvements translate into long-term patient survival and downstream treatment outcomes. Future studies will likely look at how synoptic reporting affects the speed at which patients transition from diagnosis to treatment, and whether the reduction in "surgical upstaging" (where a patient is found to have more advanced cancer during surgery than was predicted) leads to a decrease in unnecessary operations.
In the world of medical technology, we often focus on the newest imaging hardware or the latest robotic systems. However, this study serves as a powerful reminder that sometimes, the most effective "innovation" is simply a better way of organizing the information we already have. By standardizing the language of lung cancer staging, doctors are not just writing better reports—they are providing better care.