The landscape of American adolescent mental health is currently defined by a fragile paradox: while recent data indicates modest improvements in certain health outcomes, the foundational support systems for the nation’s youth are facing unprecedented political and systemic uncertainty. From the courtroom, where social media giants are being held to account for addictive design features, to the halls of Congress, where funding for critical mental health initiatives hangs in the balance, the wellbeing of the next generation has become a central, yet contentious, focus of public policy.
As the nation grapples with the lingering effects of the COVID-19 pandemic, the rise of synthetic opioids, and the ubiquity of digital life, a new analysis of 2024 data from the CDC and the National Survey on Drug Use and Health (NSDUH) reveals a population that is increasingly vulnerable, yet potentially resilient, provided that access to care is protected.
Main Facts: A Portrait of Adolescent Vulnerability
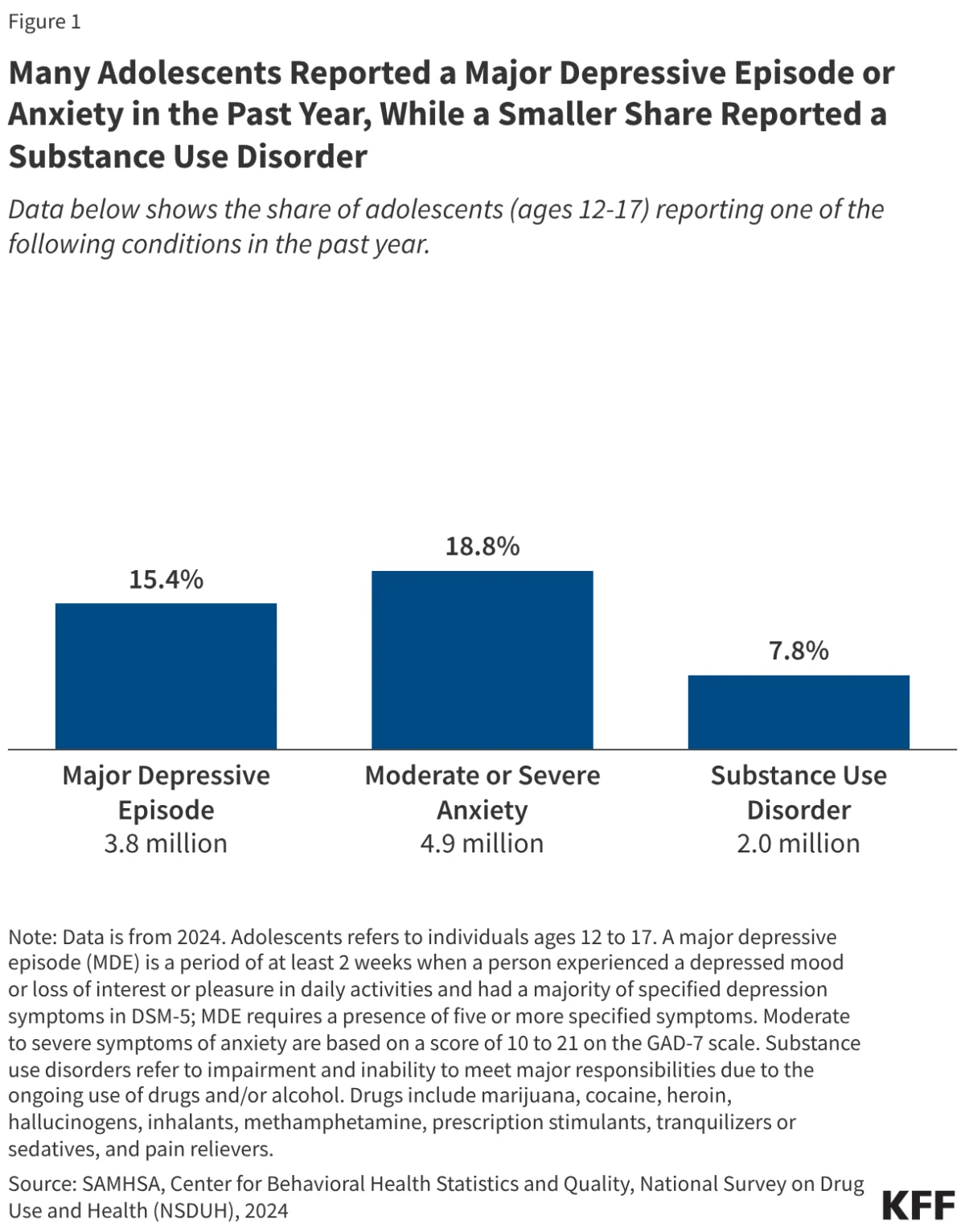
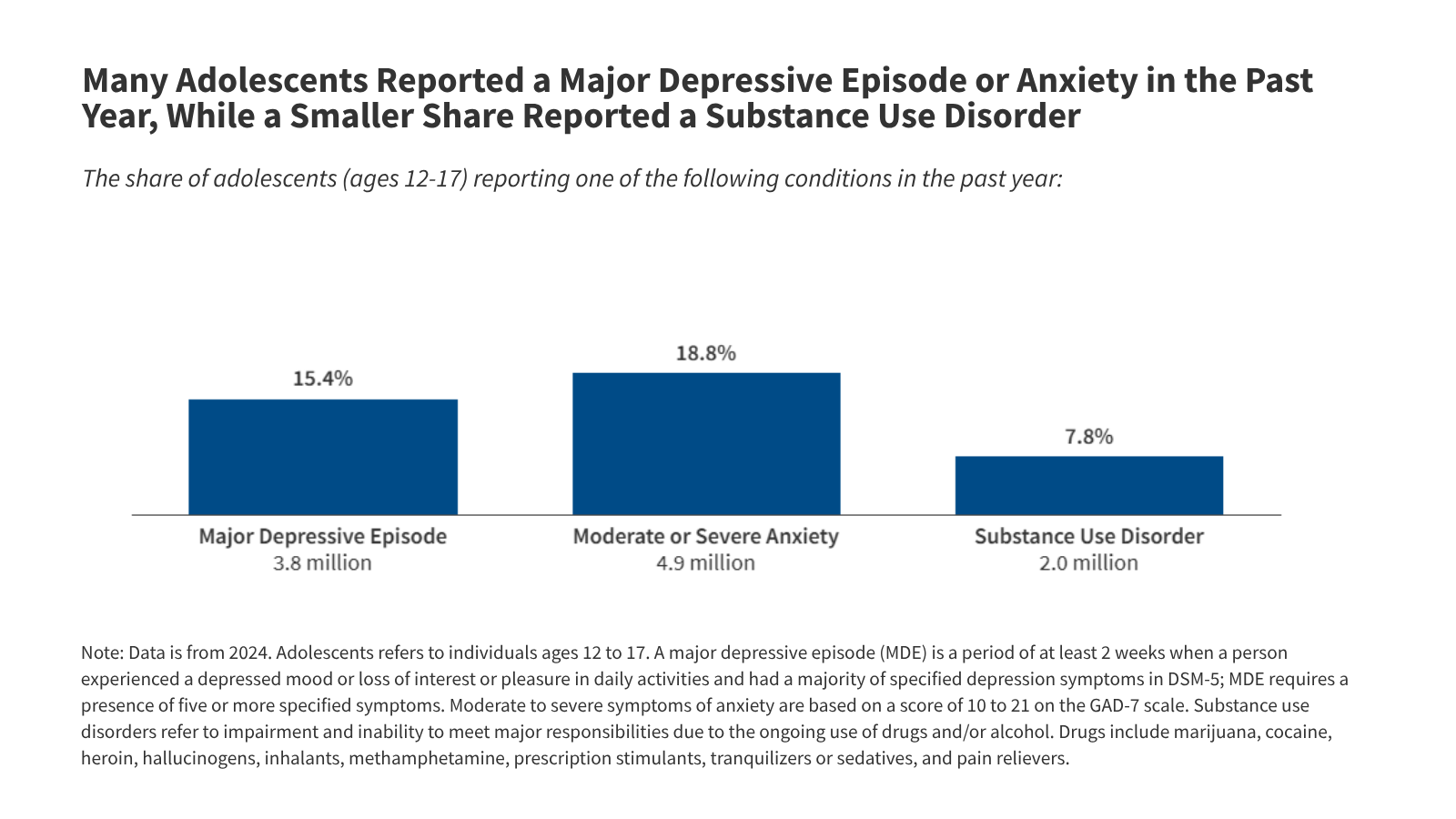
The current data presents a sobering reality. In 2024, approximately 3.8 million adolescents—roughly 15% of the population—reported experiencing a major depressive episode (MDE) within the past year. Furthermore, 19%, or 4.9 million adolescents, reported moderate to severe symptoms of anxiety. These figures, while showing a slight downward trend from the peak of the pandemic in 2021, remain significantly higher than pre-2020 baselines.
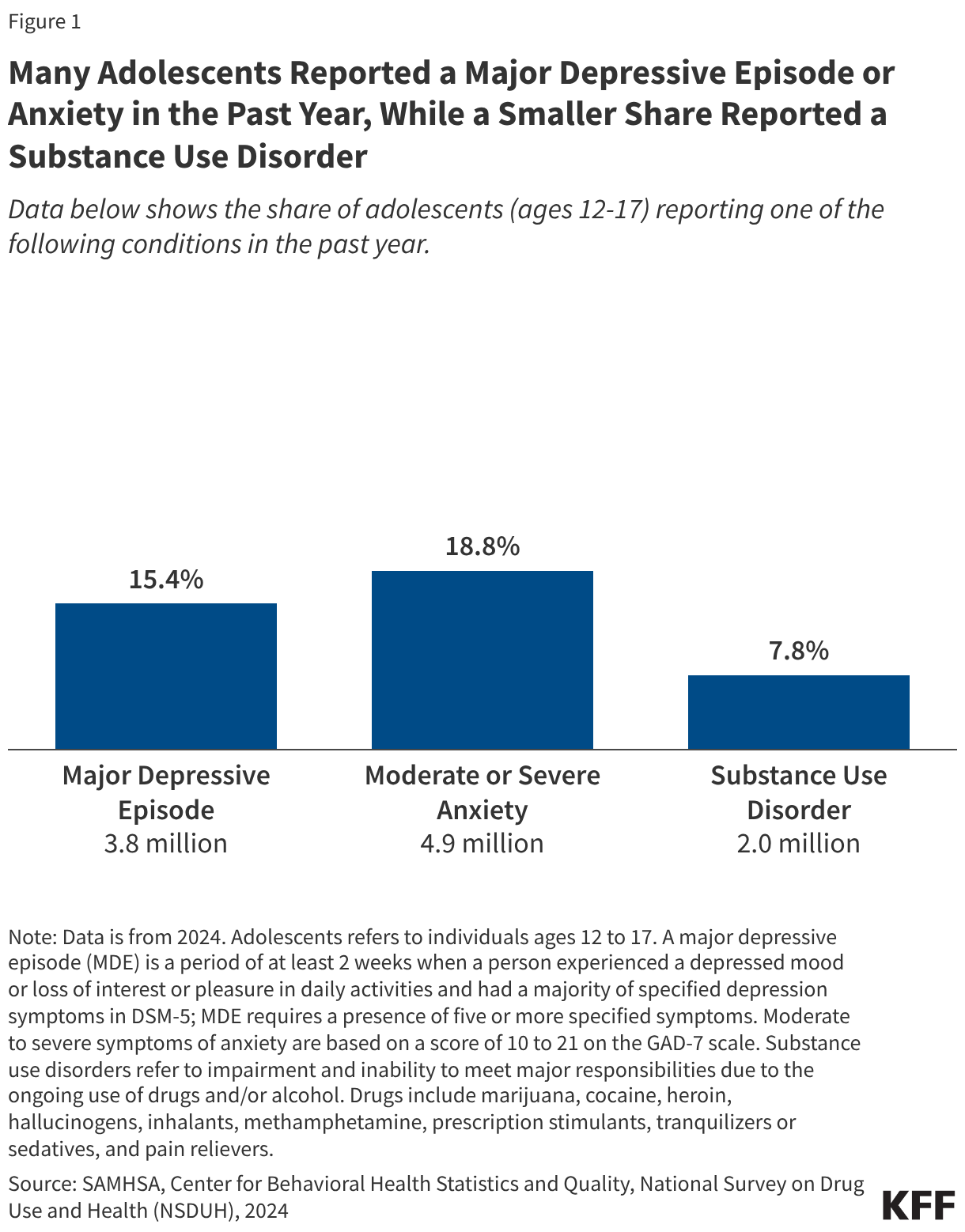
Perhaps more concerning is the inextricable link between mental health struggles and substance use. Adolescents reporting an MDE were significantly more likely to report using illicit drugs (33%) compared to their counterparts (12%). This "co-occurrence" suggests that many young people are turning to substances as a maladaptive coping mechanism for underlying psychological distress, including loneliness, trauma, and sleep deprivation.
A Chronological Perspective: From Pandemic Surge to Policy Shift
The trajectory of youth mental health over the last decade has been marked by distinct phases:
- 2013–2019 (The Pre-Pandemic Baseline): Mental health concerns were already on the rise. Feelings of sadness and hopelessness among high school students climbed from 30% to 42% over this period. Suicide rates, while fluctuating, began a steady ascent that would culminate in a peak in 2018.
- 2020–2022 (The Pandemic Catalyst): The COVID-19 pandemic acted as an accelerant for existing crises. Drug overdose deaths among adolescents more than doubled, largely driven by the infiltration of illicitly manufactured fentanyl into the youth drug supply. In 2021, the U.S. Surgeon General issued a formal advisory declaring a youth mental health crisis.
- 2022 (The Legislative Response): Congress passed the Bipartisan Safer Communities Act (BSCA), a milestone piece of legislation that directed significant federal funding toward school-based mental health services, particularly in underserved regions.
- 2023–2024 (The Current Landscape): We have witnessed a stabilization. Suicide deaths declined by 5% between 2023 and 2024, and drug overdose deaths saw a sharp, welcome drop, falling from 557 to 272 in a single year. However, this period has also seen a significant shift in federal policy, with the second Trump Administration initiating rollbacks of the very programs—such as BSCA-funded school services—that contributed to these improvements.
Supporting Data: The Intersection of Risk and Access
The data reveals that vulnerability is not distributed equally. LGBTQ youth, in particular, remain at a higher risk for suicidality, a situation exacerbated by the removal of specialized support lines, such as the dedicated extension for LGBTQ individuals within the 988 crisis network.
The Role of Substances
Marijuana has emerged as a significant factor in the clinical landscape. With its increasing legality and higher concentrations of THC, it is no longer the "soft" drug of the past. Evidence increasingly links early and frequent marijuana use to the onset of psychotic disorders, including schizophrenia. Among adolescents with an MDE, 25% report marijuana use, compared to only 8% of those without such a diagnosis.
The Impact of Firearms
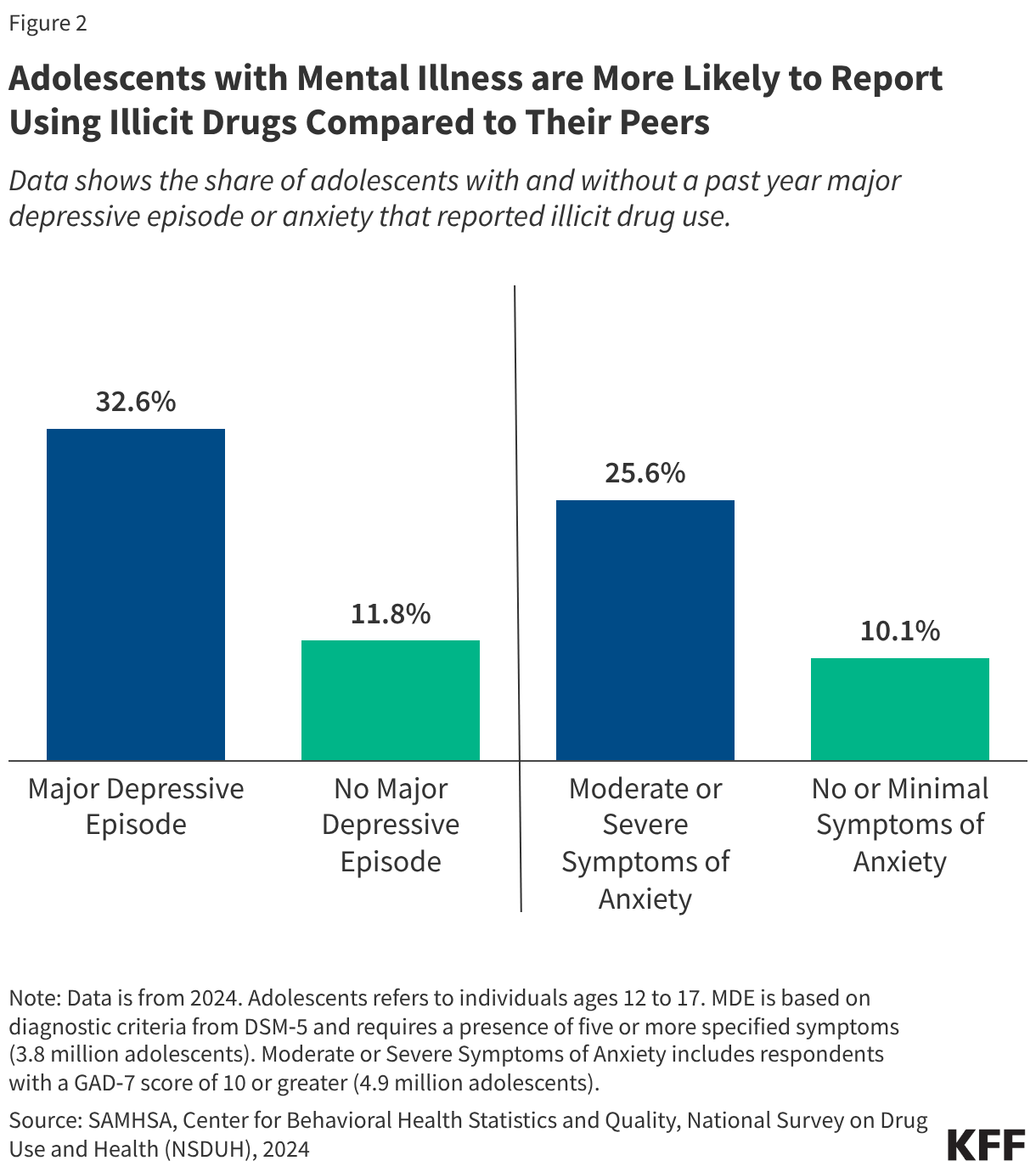
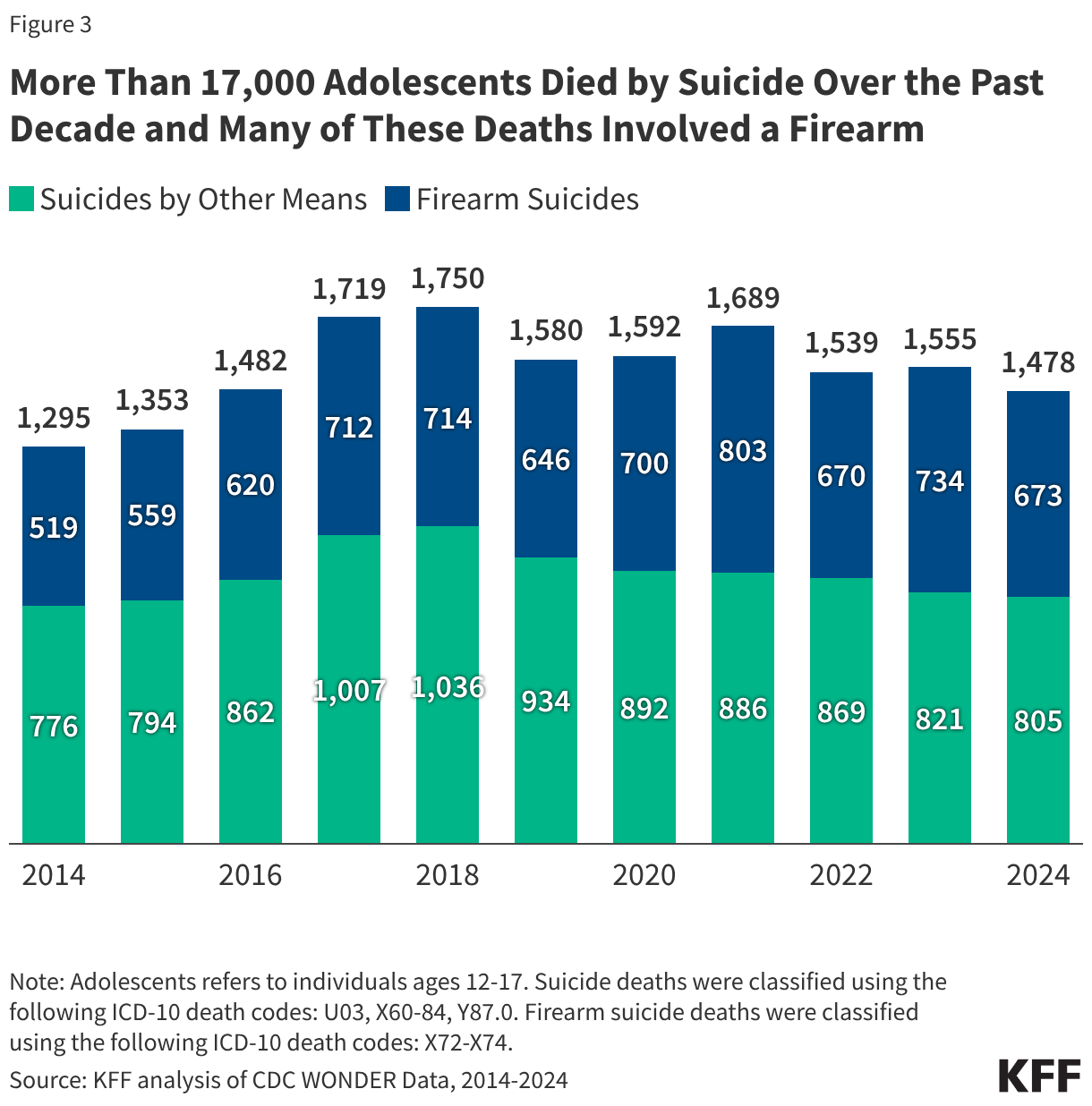
Firearms remain a primary concern for youth safety. Over the past decade, more than 17,000 adolescents have died by suicide, with more than 4 in 10 of these tragedies involving a firearm. The prevalence of unsecured firearms in homes is a direct, preventable risk factor that continues to claim young lives at a disproportionate rate.
Official Responses and Political Implications
The current federal stance toward mental health represents a stark departure from the legislative consensus of 2022. The 2027 President’s budget proposal includes substantial cuts to agencies like the Substance Abuse and Mental Health Services Administration (SAMHSA). Critics argue that these cuts, coupled with the potential restructuring of Medicaid—which covers 40% of all children and teens in the U.S.—could create a "coverage cliff."
The legal system has stepped in where policy has faltered. The landmark case of K.G.M. v. Meta Platforms, Inc. set a precedent by holding social media companies legally accountable for the mental health impacts of their algorithms. This represents a shift in the societal narrative: the blame is moving away from solely "individual" mental health struggles and toward the structural environments, including social media design and firearm accessibility, that shape adolescent behavior.
Future Implications: Can We Maintain Progress?
The decline in adolescent overdose deaths in 2024 is a testament to the effectiveness of targeted interventions. Programs like the widespread distribution of naloxone in schools and the implementation of fentanyl education reached over half of all public schools by the 2024-2025 academic year. These initiatives prove that when resources are deployed directly into the environments where adolescents spend their time, lives are saved.
However, the future remains precarious. The reliance on Medicaid as a primary payer for youth mental health services means that any contraction of this program will have immediate, negative consequences for accessibility. Furthermore, the persistent gap in treatment for substance use disorders—where only 30% of the 2.4 million adolescents in need receive care—highlights a critical infrastructure failure. Residential facilities remain prohibitively expensive and frequently lack the capacity or the clinical expertise to administer evidence-based treatments like buprenorphine to minors.
Conclusion: The Path Forward
The path to stabilizing adolescent mental health requires a multi-pronged approach that transcends party lines. If the progress of the last two years is to be maintained, policymakers must prioritize:
- Sustainable Funding: Protecting the gains made by the Bipartisan Safer Communities Act and ensuring that school-based mental health programs are not subjected to the whims of political budget cycles.
- Harm Reduction: Continuing to support initiatives like the 988 crisis hotline and widespread naloxone access, ensuring they remain inclusive and fully funded.
- Digital Responsibility: Continued regulatory and legal pressure on technology platforms to redesign features that prey on the psychological vulnerabilities of developing brains.
- Equity in Care: Expanding access to specialized, affordable residential treatment and ensuring that mental health services are integrated into the primary care settings where most adolescents receive their medical treatment.
As the nation looks toward the next decade, the evidence is clear: the mental health of our youth is not merely a private matter to be handled within the family unit. It is a public health imperative that requires a stable, funded, and compassionate commitment from the state. Without such a commitment, the hard-won improvements of 2024 risk being lost, leaving a generation to navigate an increasingly complex world without the safety nets they desperately need.