The United States stands at a precarious juncture in its approach to public health. As of 2024, the nation is grappling with a persistent and multifaceted crisis: more than 61 million American adults are navigating the complexities of mental illness, while mortality rates tied to suicide, gun violence, and drug overdoses remain at historically elevated levels. The lingering shadow of the COVID-19 pandemic—which served as a massive stress test for an already fragile healthcare infrastructure—has compounded these challenges, leaving millions of individuals struggling to access or afford the care they desperately need.
Against this backdrop, the transition to the second Trump administration in 2025 has introduced a fundamental pivot in federal strategy. While previous administrations focused heavily on expanding coverage and strengthening federal oversight, the current landscape is defined by a "law-and-order" orientation, a streamlining of federal agency roles, and a reevaluation of the government’s responsibility in funding community-based intervention.
The State of the Crisis: A Summary of Main Facts
The current mental health and substance use landscape is characterized by a "triple threat" of structural access issues, high mortality, and demographic inequality. Despite advancements in telehealth and increased awareness, the barrier to entry for mental health services remains prohibitively high for many.
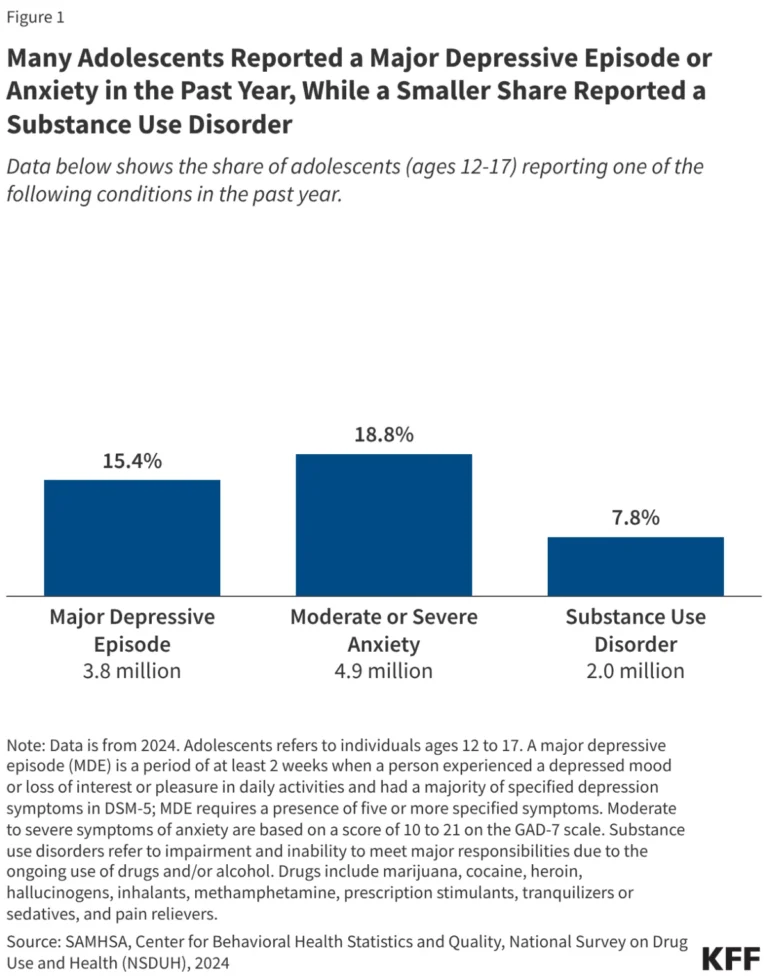
Data from the Kaiser Family Foundation (KFF) and the Substance Abuse and Mental Health Services Administration (SAMHSA) reveal a stark reality: among insured adults who self-report their mental health as "fair" or "poor," 43% reported at least one instance in the past year where they required mental health services or medication but failed to obtain them. This gap is not distributed equally. Marginalized communities—including people of color, youth, and young adults—frequently encounter systemic hurdles that prevent them from accessing care, even when they possess insurance.
The crisis is further complicated by the intersection of behavioral health with public safety. The rise in gun violence and the ongoing opioid epidemic—fueled by synthetic substances like fentanyl—have forced a national conversation about whether the government should prioritize clinical treatment, law enforcement, or a hybrid of both.
Chronology of Policy Evolution: From Expansion to Restructuring
To understand the current policy environment, one must look at the trajectory of the last decade:
- The First Trump Administration (2017–2021): The initial focus was on the legislative expansion of opioid treatment access. Key achievements included the passage of the SUPPORT Act and the creation of the 988 Suicide & Crisis Lifeline, which established a standardized, easy-to-access national system for mental health emergencies.
- The Biden Administration (2021–2025): The subsequent four years emphasized the strengthening of SAMHSA, the expansion of healthcare coverage under the Affordable Care Act, and the implementation of evidence-based, clinically driven treatment programs. By mid-2023, these efforts saw some stabilization in opioid-related deaths, though progress remained uneven.
- The Second Trump Administration (2025–Present): The current administration has initiated a significant reversal. While maintaining some continuity with established opioid treatment laws, the executive branch has shifted toward a more restricted, centralized, and security-oriented model of management.
Supporting Data and Evidence: The Pulse of Public Health
The effectiveness of these policies is measured through a complex array of indicators. Prior to the 2025 policy shift, the expansion of federal funding for mental health grants in schools and community-based violence intervention programs was credited with filling significant "care deserts."
However, the current administration’s move to reorganize federal infrastructure—specifically proposals to reduce the independent reach of SAMHSA—has sparked debate among policy analysts. Proponents argue that streamlining federal bureaucracy increases accountability. Conversely, public health experts point to the 43% "unmet need" rate among insured individuals as proof that any reduction in federal oversight could exacerbate existing inequities. The data indicates that when federal guidance is inconsistent or when grant programs (such as those for school-based mental health) are canceled, the downstream effect is a lack of localized support for the most vulnerable populations, particularly youth and young adults.

Official Responses and Strategic Shifts
The second Trump administration has been clear about its ideological alignment with proposals found in the Project 2025 mandate. The strategy is characterized by four primary pillars:
- Legislative Hardening: The signing of the HALT Fentanyl Act represents a move toward stricter criminal penalties and supply-side interdiction. This shift favors a law-and-order approach over purely clinical, harm-reduction models.
- Fiscal Consolidation: By restructuring SAMHSA and proposing the reduction of federal leadership capacity in mental health, the administration aims to return more decision-making power to state governments.
- Selective Funding: The administration has signaled a pivot away from "soft" interventions. A prime example is the rescinding of certain community violence intervention grants, which the White House argues should be handled through local law enforcement rather than federal social services.
- Continuity of Core Treatment: Despite the broader shift, the administration has maintained a commitment to the reauthorization of the SUPPORT Act, suggesting that while the method of delivery is changing, the necessity of opioid treatment remains a bipartisan pillar of the federal agenda.
Implications: The Future of Care
The shift in federal policy has profound implications for the American public. As the administration moves toward a decentralized, security-focused model, the responsibility for mental health and substance use disorder treatment is increasingly being shifted to state and local entities.
Impact on Marginalized Communities
The primary concern among health equity advocates is that the reduction in federal funding for school-based programs and community violence interventions will disproportionately impact youth in low-income urban and rural areas. Without federal grants, these communities may be unable to maintain the infrastructure necessary to prevent crises before they escalate into violence or overdose.
The Access Gap
The "access gap" remains the most critical metric for the coming years. If the federal government reduces its role in guiding insurance standards and mental health parity, the burden on the private insurance market will increase. If the private sector fails to close the 43% unmet need gap, the number of individuals entering the criminal justice system due to untreated mental illness may rise, effectively forcing the prison system to serve as the nation’s de facto mental healthcare provider.
The Long-term Outlook
The effectiveness of the "law-and-order" approach to the opioid epidemic will be tested in the coming 24 months. If the HALT Fentanyl Act succeeds in curbing supply, the administration may claim a victory in public safety. However, if the simultaneous reduction in support services leads to a spike in recidivism or an increase in untreated addiction among those who do not respond to interdiction, the administration may face significant political and social backlash.
A Tracker for a Changing Landscape
To assist policymakers, researchers, and the public in navigating these shifts, a new tracking tool has been developed. This tracker serves as a living repository of the second Trump administration’s actions, categorized into four distinct streams:
- Opioids and Substance Use: Monitoring the implementation of new legislative mandates and the status of existing treatment programs.
- Mental Health: Tracking the impact of reduced federal grant support and the reorganization of school-based services.
- Federal Infrastructure: Documenting the restructuring of SAMHSA and other health-related agencies.
- Gun Violence: Cataloging the impact of policy changes on community-level intervention funding.
As the nation moves forward, the success of these policies will not be measured solely by legislative passage, but by the tangible health outcomes of the 61 million Americans currently affected by mental illness. The shift in 2025 marks more than just a change in administration; it marks a fundamental debate over whether the federal government should act as a safety net for the vulnerable or as a regulator of public order. The next few years will provide the data necessary to determine which path best serves the American people.