In the daily practice of restorative and prosthetic dentistry, few tools are as ubiquitous—or as deceptively simple—as articulating paper. For decades, clinicians have relied on these thin, inked strips to identify where teeth meet, adjusting occlusal surfaces to ensure patients can chew comfortably and effectively. Yet, despite its status as a staple of modern dental care, the accuracy of this low-cost, high-speed method has often been debated.
A groundbreaking clinical study, published in the May 2026 issue of the journal Diagnostics, has finally provided a rigorous assessment of how to optimize the use of articulating paper. Led by researchers from the University of Barcelona and the Bellvitge Biomedical Research Institute (IDIBELL), the study challenges long-held clinical assumptions and offers evidence-based recommendations for improving the precision of occlusal analysis.
Main Facts: The Reality of "Blue Marks"
The study, titled "Clinical Strategies to Improve the Accuracy of Articulating Paper for Detecting Occlusal Contact Points in Adults with Natural Dentitions," sought to quantify the validity of articulating paper by comparing it against a "gold standard": silicone occlusal registrations analyzed via high-resolution digital software.

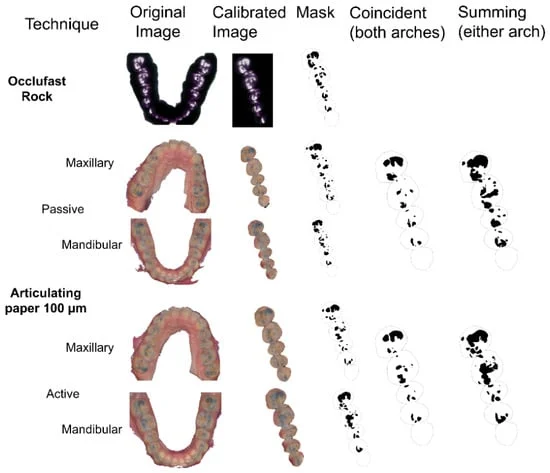
The researchers analyzed 32 adult participants with healthy natural dentitions, examining variables including paper thickness (100 µm vs. 200 µm), clinical technique (passive holding vs. active pulling), and the choice of dental arch (maxillary vs. mandibular).
The findings were striking:
- Overall Accuracy: Articulating paper correctly identified 81% of true occlusal contact points.
- The False-Positive Problem: Approximately 15% of the marks left by the paper were false positives—meaning they indicated contact where none actually existed.
- The Cusp-Tip Trap: A significant two-thirds of these false-positive marks were located specifically on the tips of cusps. Researchers concluded these are likely "artifactual" marks caused by the paper rubbing against the prominent cusp tips during the patient’s closing movement.
- The Thickness Factor: Contrary to the belief that thinner is always better, the study found that 200 µm paper resulted in significantly fewer false-positive marks (9.4%) compared to the 100 µm paper (20.6%).
Chronology of the Research Process
The investigation was a multi-year effort that prioritized clinical rigor and statistical power.

- July 2020: The study protocol received official approval from the Ethics Committee of the Barcelona University Dental Hospital.
- Clinical Phase: The research team, led by Dr. Bernat Rovira-Lastra, conducted a cross-sectional test-retest study. Each participant underwent multiple recording sessions to ensure reproducibility.
- Analysis Phase: Using FIJI software (ImageJ), the team performed complex digital transformations, calibrating the articulating paper marks against the silicone reference standard. This allowed for a precise pixel-by-pixel comparison.
- Retesting: To ensure the reliability of the findings, the entire clinical procedure was repeated for each participant two weeks after the initial session.
- May 2026: Following a peer-review process, the results were formally published in Diagnostics, establishing new benchmarks for clinical occlusal assessment.
Supporting Data: Why Technique Matters
The data gathered in this study provides a roadmap for practitioners who want to reduce errors in their restorative workflows. One of the most significant takeaways involves the "Arch Selection" strategy.
The study found that the mandibular arch is more conducive to accurate assessment, yielding a higher percentage of true-positive contacts compared to the maxillary arch. Furthermore, when clinicians adopted a "Coincidence Protocol"—only marking an occlusal contact as "true" if the blue marks aligned on both the maxillary and mandibular arches—the false-positive rate plummeted to just 2%.
Regarding the "pulling" technique (where the clinician pulls the paper out from between the teeth as the patient closes), the study found no statistical evidence that this improves diagnostic accuracy. This suggests that the extra effort involved in the pulling method may not be necessary for achieving a reliable result, provided the clinician ensures the paper is placed properly and the patient is firmly in the intercuspal position.

Official Perspectives and Clinical Implications
Dr. Jordi Martinez-Gomis, the corresponding author of the study, emphasizes that while digital systems like T-Scan or intraoral scanners are increasingly popular, the reality of clinical practice keeps articulating paper at the forefront of dentistry.
"Articulating paper remains the most widely used method because of its cost-effectiveness and speed," the authors noted in their discussion. "However, the clinical subjectivity of interpreting these marks has always been a limitation. Our goal was to provide evidence that allows a general practitioner to move from ‘eyeballing it’ to a more scientific approach."
Implications for the Future of Dentistry
- Standardizing Clinical Guidelines: The study highlights the urgent need for a standardized approach to occlusal analysis. The researchers suggest that rather than guessing, dentists should verify contact points by observing the match between the maxillary and mandibular arches.
- Refining Material Choices: The evidence favoring 200 µm paper for reducing false-positive cusp-tip marks is a call for practitioners to re-evaluate the inventory in their clinics.
- The Role of AI: The authors acknowledge that the next phase of this research will likely involve artificial intelligence. By training algorithms to recognize the difference between "true" contact signatures and "rubbing" artifacts on cusp tips, the diagnostic power of articulating paper could be boosted even further.
- A Call for Further Research: While this study focused on healthy natural dentitions, the team acknowledged that the results cannot be immediately extrapolated to patients with complex prostheses or severe occlusal disorders. Future research must expand the scope to include patients with crowns, bridges, and implants.
Conclusion: A More Precise Path Forward
The study from the University of Barcelona is a significant contribution to dental science because it validates a "low-tech" tool using "high-tech" methodology. It demonstrates that the problem with articulating paper is rarely the paper itself, but rather the human error in interpreting the marks it leaves behind.

By shifting clinical habits—specifically, by favoring 200 µm thickness, focusing on the mandibular arch, and ignoring isolated marks on cusp tips that do not have an antagonist match—dentists can significantly improve the accuracy of their occlusal adjustments. This not only leads to better patient comfort but also improves the longevity of restorative work. As the dental profession continues its rapid digital transformation, this study serves as a critical reminder that even the simplest tools, when used with scientific rigor, remain essential to the art and science of dentistry.
Reference:
Rovira-Lastra, B.; ElOtmani-Sabiri, S.; Ustrell-Barral, M.; Khoury-Ribas, L.; Martinez-Gomis, J. "Clinical Strategies to Improve the Accuracy of Articulating Paper for Detecting Occlusal Contact Points in Adults with Natural Dentitions." Diagnostics 2026, 16(10), 1450. https://doi.org/10.3390/diagnostics16101450