For decades, the oncology community has grappled with a persistent and frustrating reality: while researchers have made massive strides in killing cancer cells, the debilitating side effects of those treatments remain stubbornly difficult to prevent. Among the most common and life-altering is chemotherapy-induced peripheral neuropathy (CIPN)—a condition characterized by numbness, tingling, and chronic pain that can affect up to 80% of patients receiving common chemotherapy agents like taxanes and platinum analogs.
Yet, despite years of rigorous clinical research, no standard, effective intervention has emerged to prevent CIPN. Now, a new meta-analysis published in the journal Cancers suggests that the reason for this failure may not lie entirely with the drugs being tested, but with a complex, often overlooked ghost in the machine: the placebo effect.
The Trigger: The Duloxetine Disappointment
The investigation into the "placebo problem" was sparked by a recent high-profile, multisite clinical trial funded by the National Cancer Institute (NCI). The study aimed to test the efficacy of duloxetine—a serotonin-norepinephrine reuptake inhibitor (SNRI) known for its pain-relieving properties—in preventing CIPN before it took hold in patients.
The results were, by all accounts, perplexing. Rather than seeing a clear divide between the treatment group and the placebo group, researchers found almost uniform success across the board. Approximately 65% to 68% of participants in every group—whether they received the drug or a sugar pill—reported little to no neuropathy.

This near-equivalent response rate across the arms of the trial suggested that the "placebo response" was not just a minor variable, but a potentially overwhelming factor that could be masking the actual efficacy of the drug. If a placebo is performing as well as a potent pharmaceutical, the trial design is essentially rendered powerless to distinguish the two.
A Chronology of Clinical Stagnation
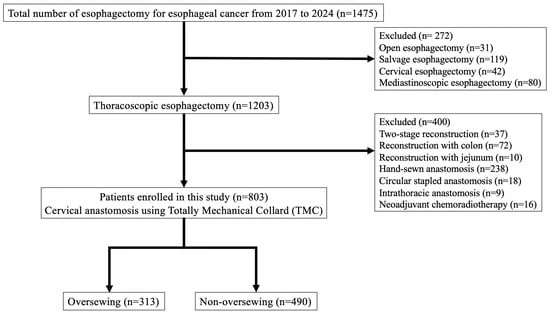
To understand if this phenomenon was a one-off anomaly or a systemic issue, researchers at the Mayo Clinic and the University of Alabama at Birmingham conducted a meta-analysis of seven randomized, double-blinded, placebo-controlled trials conducted over the last 20 years.
- 2014–2019: The era of testing various agents like Glutathione, Pregabalin, and Minocycline. Across these trials, researchers consistently struggled to move the needle on CIPN prevention, often reporting inconclusive data.
- 2020: The American Society of Clinical Oncology (ASCO) releases a guideline update, highlighting the lack of progress in CIPN prevention and the failure of existing trials to find a gold-standard intervention.
- 2023: The conclusion of the multi-site NCI-funded duloxetine study (Alliance A221805), which provided the patient-level data necessary to begin a deeper dive into the placebo effect.
- March 2026: The current study is submitted for peer review, marking a shift in focus from "which drug works" to "why our trials are failing to show what works."
- May 2026: The meta-analysis is published, offering a roadmap for future clinical trial designs.
Dissecting the Data: The Weight of Expectations
The research team, led by David Zahrieh and Ellen M. Lavoie Smith, pooled data from 191 participants across seven trials. They categorized "response" in two ways: a conservative definition (reporting "not at all" for neuropathy symptoms) and a broader definition (reporting "not at all" or "a little").
The meta-analysis revealed that the placebo response rate varied wildly depending on the strictness of the definition—ranging from 10% to nearly 40%. While 40% is high, it is not unheard of in pain-related research. However, the data revealed specific, statistically significant predictors for higher placebo responses that should alarm researchers:

- Gender Dynamics: Male participants were significantly more likely to report a "placebo response" than female participants.
- Drug Type: Patients receiving oxaliplatin exhibited higher placebo response rates than those receiving paclitaxel.
- Randomization Ratios: Perhaps most critically, trials that used a 2:1 randomization ratio (favoring the experimental drug) saw higher placebo responses than those with a 1:1 ratio. This suggests that simply knowing they have a higher statistical chance of receiving the active drug may prime the patient’s psychological state, leading to a heightened perception of symptom improvement.
The "Invisible" Factors
Beyond the statistics, the researchers hypothesize that human elements—optimism, desperation, and intensive patient support—are acting as massive, unmeasurable confounders.
In the duloxetine trial, for instance, a dedicated nurse liaison was assigned to support the participating sites. While this individual provided vital care and education, the researchers suggest that this level of dedicated, warm, and constant human contact may have inadvertently created an environment of high expectation. When patients feel "cared for" and "supported" by a professional who is clearly invested in their success, their physiological perception of pain often shifts.
Furthermore, the "desperation factor" cannot be ignored. After decades of failures, both the research staff and the patients are acutely aware of the lack of solutions for CIPN. This shared hope—that "this time, it will be different"—is a powerful psychological force that can manifest as a real, measurable reduction in reported symptoms in a clinical setting.
Official Perspectives and Implications
The study authors are careful to note that their findings are not a critique of the investigators or the trials themselves, but rather a call to arms for better methodology. "High placebo response rates can threaten scientific progress," the study concludes.

The implications are immediate for future trial design:
- Stricter Definitions: Researchers may need to shift toward more objective, potentially digital or biomarker-based measurements of neuropathy rather than relying solely on subjective patient-reported outcomes like the EORTC QLQ-CIPN20.
- Trial Design Reform: The use of unequal randomization ratios (like 2:1) might need to be reconsidered if they are proven to artificially inflate patient expectations and, by extension, the placebo effect.
- Managing Expectations: Standardizing how the trial is explained to patients to ensure that "hope" does not transition into "expectation of cure" may be necessary.
The Path Forward
The quest to solve CIPN is not just about finding the right molecule; it is about refining the scientific lens through which we view human suffering. If the medical community continues to ignore the placebo effect, they risk discarding potentially life-saving treatments simply because they cannot prove their efficacy against the powerful, psychological noise of the clinical trial environment.
By identifying the predictors of the placebo response—gender, chemotherapy agent, and trial structure—the researchers have provided a diagnostic tool for future trials. The next step, according to the study’s conclusion, is to integrate this knowledge into the very architecture of cancer research. Only by minimizing the psychological "noise" can the signal of a truly effective treatment finally be heard.
As the oncology field looks toward the next decade of research, the lesson of 2026 is clear: the patient’s mind is as much a part of the treatment as the drug itself, and it is time to start measuring that impact with the same rigor as any other chemical compound.