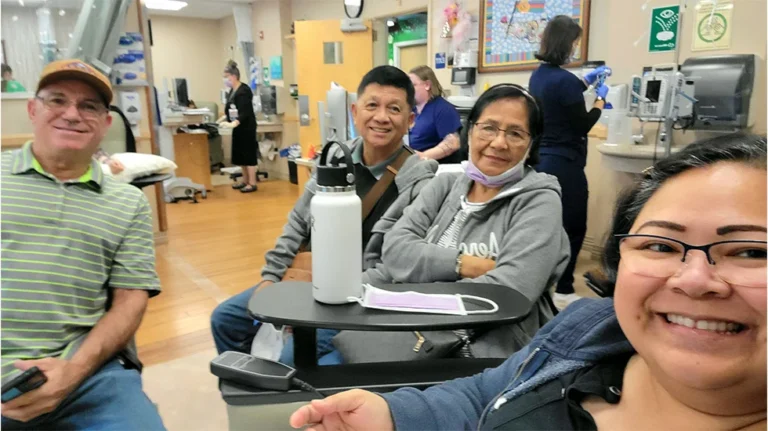
This feature was developed in collaboration with Gina Franco, MSN, NP-C, Dip ACLM, Director of the Center for Integrative Oncology & Survivorship and Director for Cancer Prevention and Wellness at Prisma Health Institute in Greenville, South Carolina.
A breast cancer diagnosis is a life-altering event that radiates through every facet of a woman’s existence. Beyond the rigorous demands of clinical treatment, patients often face profound shifts in their self-perception, their relationship with their own body, and the dynamics of their intimate connections. While often overshadowed by the urgent need to address the disease, sexual health is a vital component of quality of life—one that frequently suffers during and after treatment.
It is essential to state clearly: changes in sexual health are not a personal failure. They are a common, documented biological and psychological response to the trauma of cancer treatment. With time, specialized support, and the right clinical tools, many women find a path toward renewed confidence, connection, and physical pleasure.
The Reality of Sexual Dysfunction in Survivorship
Sexual health after breast cancer is not a "one-size-fits-all" experience. However, the prevalence of these challenges is statistically significant. Recent data suggests that nearly 90% of breast cancer patients report moderate-to-severe changes in their sexual lives following their treatment protocols.

In clinical terms, when these changes cause distress or dysfunction, it is categorized as "Female Sexual Dysfunction." This is not merely a lack of desire; it encompasses a spectrum of persistent physical and emotional alterations, including decreased libido, difficulty achieving arousal, persistent pain during intercourse (dyspareunia), and changes in the experience of orgasm.
The Biological and Psychological Interplay
The causes of these challenges are twofold. Physically, treatments such as surgery, chemotherapy, radiation, and hormonal therapies induce systemic changes. Chemotherapy, for instance, can force the ovaries into premature menopause, causing an immediate drop in estrogen that directly affects vaginal tissue health and sexual desire.
Psychologically, the diagnosis often triggers a sense of body betrayal. Scars from surgery, hair loss, or changes in breast shape can lead to diminished self-esteem. When these physical changes are coupled with the anxiety and depression that often accompany a cancer journey, the result is a significant barrier to intimacy.
Chronology: Understanding Treatment Impacts
To manage sexual health effectively, patients must understand how specific treatments influence their bodies. While side effects vary by individual, they typically follow the timeline of treatment intervention.

Surgical Impact
Surgery, whether a lumpectomy or mastectomy, often results in physical scarring and potential nerve damage. This can lead to a loss of sensation in the breast or nipple, forcing a woman to rethink how she perceives her own body as a source of pleasure. Emotional processing of these changes is a critical step in the post-surgical recovery phase.
The Chemotherapy Experience
Chemotherapy interferes with hormone regulation. By suppressing ovarian function, it can trigger premature menopause. Symptoms such as hot flashes, extreme fatigue, and severe vaginal dryness are common. For many, this menopause is temporary, but for others, it is a permanent change that requires long-term management strategies.
Radiation and Skin Sensitivity
Radiation therapy to the chest wall can cause localized skin irritation and tissue tightening. This can make physical contact uncomfortable and may require specific skin-care protocols recommended by a radiation oncologist to maintain comfort.
The Long-Term Commitment: Hormonal Therapy
For patients with hormone receptor-positive (HR+) breast cancer, hormonal therapy (such as Tamoxifen or aromatase inhibitors) is often prescribed for 5 to 10 years. While these drugs are life-saving and crucial for preventing recurrence, they are notoriously difficult regarding sexual side effects, including severe dryness and libido loss. It is critical that patients do not discontinue these medications without consulting their physician. Instead, patients should request active management strategies for these side effects.

Supporting Data: Why Clinical Intervention Matters
The medical community has shifted its stance on "living with" these side effects. The American Urological Association (AUA), in conjunction with several international medical societies, released updated guidelines in 2025 regarding Genitourinary Syndrome of Menopause (GSM).
The data confirms that for many survivors, non-hormonal, over-the-counter interventions—such as high-quality, water-based lubricants and vaginal moisturizers—are the first line of defense. However, when these are insufficient, the guidelines now support a nuanced, shared-decision-making process between the oncologist and the gynecologist to determine if low-dose vaginal estrogen is safe and appropriate for the individual patient. This represents a significant evolution in care, moving away from the "nothing can be done" narrative.
Official Perspectives: The Role of the Care Team
Gina Franco and other leading oncological experts emphasize that silence is the enemy of recovery. Patients should never feel that sexual health is a "taboo" topic to bring up during an oncology follow-up.
Recommended Clinical Strategies
- Pelvic Floor Physical Therapy: Many survivors experience pelvic floor tension due to pain and anxiety. A specialized therapist can teach relaxation and strengthening techniques that significantly reduce pain during intimacy.
- Non-Hormonal Drug Therapies: There are FDA-approved non-hormonal medications designed to address low libido by acting on neural pathways rather than hormones.
- Counseling: Whether individual or couples-based, therapy provides a safe space to navigate the grief and body-image changes that accompany a diagnosis.
Practical Implications for Reconnecting
Reconnecting with one’s body is a process of "re-learning." After treatment, the body may feel like a foreign landscape. To navigate this:

- Expand the Definition of Intimacy: Shift the focus away from penetrative intercourse, which may be painful, toward other forms of connection. Cuddling, massage, or simply holding hands can help bridge the gap.
- Utilize Assistive Devices: Clitoral stimulators and vibrators can aid in achieving arousal and pleasure. These are legitimate medical tools for recovery and can be discreetly sourced.
- Mindful Practices: Yoga, meditation, and journaling help to ground the patient in the present moment, moving the mind away from the "cancer-patient" identity and back into a state of self-possession.
When to Seek Immediate Help
Patients should proactively contact their healthcare provider if they notice:
- Unexplained or persistent pelvic pain.
- Signs of infection (fever, unusual discharge, or burning).
- Symptoms of severe depression or suicidal ideation.
- Bleeding during or after intercourse.
Conclusion
The path to restoring sexual health after breast cancer is neither linear nor immediate. It requires patience, open communication with partners, and a proactive relationship with a medical team. By validating these challenges as a normal part of the survivorship journey, women can transition from a place of fear and disconnection to a place of agency and renewed intimacy. You are not alone in this; there is a wealth of resources, specialized medical professionals, and supportive communities ready to help you navigate this final, vital chapter of your recovery.
For more information on support groups, patient navigators, and educational resources, visit the National Breast Cancer Foundation’s portal to ensure you have the support you need as you navigate life after cancer.