Istanbul, Turkey – [Date of Publication] – A pioneering study conducted by researchers at Acibadem Mehmet Ali Aydinlar University has unveiled promising findings regarding the efficacy of Manual Lymph Drainage (MLD) in alleviating breast edema, a common and often debilitating side effect following breast-conserving surgery and radiotherapy. The research, published in the esteemed journal Cancers, suggests that integrating MLD into standard post-treatment care can significantly improve patient outcomes, offering a new ray of hope for breast cancer survivors.
Key Findings: MLD Offers Tangible Relief for Breast Edema
The study, a preliminary randomized controlled trial, investigated the impact of adding MLD to conventional treatment protocols, which typically include education, compression therapy, and exercise. The results indicate a clear advantage for patients who received MLD alongside standard care. These individuals reported substantial improvements in key areas such as breast pain, swelling, and overall quality of life, surpassing those who received only standard care.
"Breast edema, while often overshadowed by other treatment side effects, can profoundly impact a patient’s physical comfort, body image, and emotional well-being," stated Dr. Nuray Alaca, lead author of the study and a prominent figure in physiotherapy and rehabilitation at Acibadem Mehmet Ali Aydinlar University. "Our findings provide compelling evidence that Manual Lymph Drainage can be a valuable adjunct to existing rehabilitation programs, offering tangible relief and enhancing the recovery journey for breast cancer survivors."
A Chronology of Treatment and Recovery
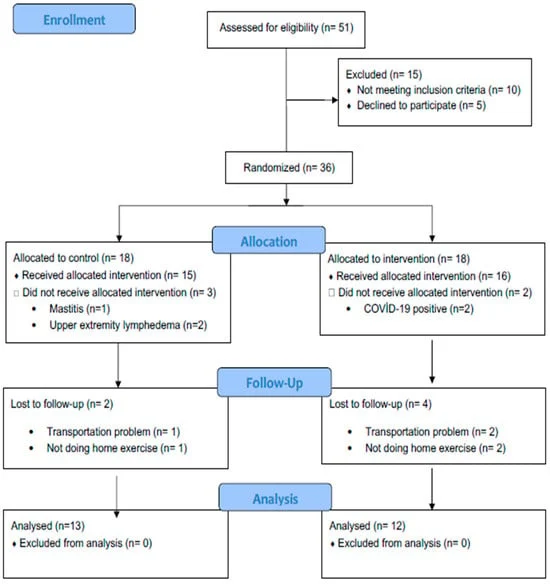
The research involved 25 female participants who had undergone breast-conserving surgery and adjuvant radiotherapy. Participants were assigned to either a control group, receiving standard care, or a treatment group, which included MLD in addition to standard care. Assessments were conducted immediately after radiotherapy and again three months post-treatment.

The study meticulously tracked several variables, including general body pain, fatigue, breast pain, breast edema severity, anxiety, depression, and quality of life. The findings revealed that while both groups experienced improvements in many of these areas, the treatment group consistently demonstrated superior outcomes. Specifically, the addition of MLD led to:
- Reduced Breast Pain: Patients receiving MLD experienced a significantly greater reduction in breast pain compared to the control group.
- Alleviated Breast Swelling: Objective and subjective measures of breast edema showed marked improvement in the MLD group.
- Improved Quality of Life: Several quality-of-life indicators, including global health status, fatigue, pain, and breast and arm symptom management, were significantly better in the treatment group.
- Enhanced LENT-SOMA Criteria: The LENT-SOMA criteria, a system for assessing late effects of radiotherapy, indicated greater improvements in pain, fibrosis, edema, retraction, and skin pigmentation in patients who received MLD.
Supporting Data: Quantifying the Benefits of MLD
The study’s detailed statistical analysis provides robust support for the observed benefits. For instance, breast pain scores in the treatment group dropped from a baseline average of 9.17 to a remarkable 1.50 after three months, a reduction of over 7.6 points on the Visual Analog Scale (VAS). In contrast, the control group saw a reduction from 7.69 to 5.54, a difference of 2.15 points. Similar significant discrepancies were noted in breast edema measures, where the Breast Edema Questionnaire (BrEQ) scores decreased by an average of 6.70 points in the treatment group versus 2.21 points in the control group.
Furthermore, the quality of life assessments painted a clear picture of improved well-being. The EORTC QLQ-C30 global health scale, a key indicator of overall quality of life, showed a substantial improvement of 56.90 points in the MLD group, compared to 40.40 points in the control group. The EORTC QLQ-BR23, which focuses on breast cancer-specific quality of life, highlighted significant gains in managing systemic therapy side effects, breast symptoms, and arm symptoms for patients receiving MLD.
Official Responses and Expert Opinions
The publication of these findings has generated considerable interest within the medical community. Experts are highlighting the importance of this research in addressing a previously under-researched area of breast cancer survivorship.

"This study is a crucial step forward in understanding how to best manage breast edema," commented Dr. Cihan Uras, a contributing author and a General Surgery specialist. "The fact that we observed such positive results, even with a preliminary study design, underscores the potential of MLD as a standard component of care. It’s vital that we continue to explore and validate these findings to offer the best possible support to our patients."
The study’s authors emphasize that while the results are highly encouraging, they are preliminary. They call for larger, multicenter randomized controlled trials with blinded assessments and objective outcome measures to further solidify these findings and fully isolate the independent effect of MLD.
Implications for Patient Care and Future Research
The implications of this study are far-reaching. Breast edema can significantly impede a patient’s return to daily activities, affect their self-perception, and contribute to psychological distress. By demonstrating the effectiveness of MLD, this research opens doors for improved rehabilitation protocols that can enhance the quality of life for a substantial number of breast cancer survivors.
The researchers acknowledge the limitations of their study, including the small sample size and the lack of blinding for practitioners and patients. However, they assert that the consistent improvements observed across multiple outcome measures, particularly in areas like breast pain and edema, warrant serious consideration for the inclusion of MLD in clinical practice.

The study also highlights the need for continued investigation into the underlying mechanisms of breast edema and the precise role of MLD in its management. Future research could explore optimal MLD techniques, treatment duration, and patient selection criteria to maximize therapeutic benefits. The findings serve as a strong impetus for further research, aiming to establish MLD as an evidence-based, integral part of comprehensive breast cancer rehabilitation.