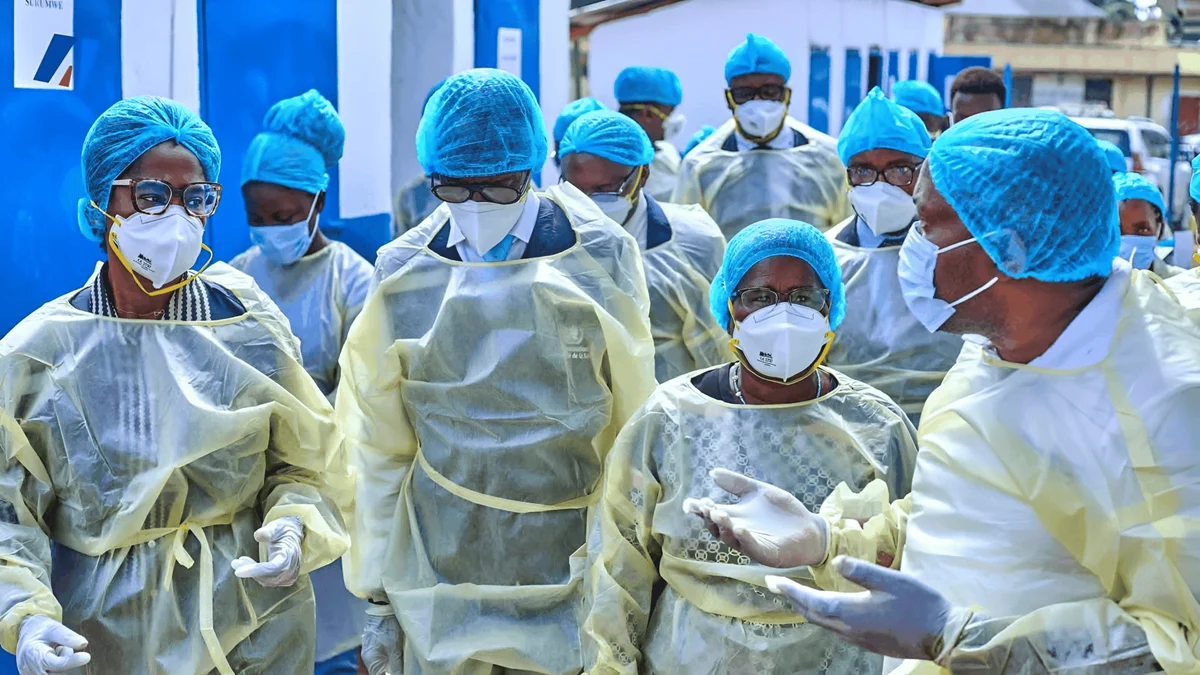
In an era defined by the rapid emergence of novel pathogens and the increasing interconnectedness of global travel and trade, the World Health Organization (WHO) has underscored a critical truth: pandemic preparedness is not merely a national responsibility, but a global imperative. On April 22 and 23, the international health community concluded "Exercise Polaris II," a sophisticated, high-level simulation designed to stress-test the world’s collective defenses against a rapidly spreading, fictional bacterial threat.
The two-day operation saw the mobilization of 26 countries and territories, 600 frontline health emergency experts, and over 25 international partners. By operating under simulated “real-life” conditions, the exercise served as a crucible for the Global Health Emergency Corps (GHEC), evaluating how nations coordinate their emergency workforces, share vital epidemiological data, and align policies in the face of an existential health crisis.
The Architecture of the Simulation: Testing Global Readiness
Building upon the foundations laid by "Polaris I"—a similar simulation conducted in April 2025 that focused on a viral threat—Polaris II escalated the complexity of the scenario. While Polaris I established the baseline for international cooperation, Polaris II was designed to operationalize specific, recently adopted frameworks.
The exercise focused on two primary pillars:
- The Global Health Emergency Corps (GHEC) Framework: Adopted in June 2025, this framework emphasizes sovereignty, equity, and solidarity. It seeks to standardize how personnel are deployed across borders, ensuring that when a region is overwhelmed, support is not just available, but effectively integrated into the local response structure.
- The National Health Emergency Alert and Response Framework: Published in October 2025, this roadmap provides the essential nuts and bolts for local, sub-national, and national coordination.
During the 48-hour event, participating nations activated their emergency coordination centers. They were tasked with managing the surge of a fictional pathogen, necessitating the rapid exchange of clinical data and the deployment of specialized health teams. Crucially, the simulation integrated AI-enabled tools for workforce management and strategic planning, marking a significant step forward in the use of predictive analytics for public health crisis management.
Chronology of the 48-Hour Operation
Day One: Detection and Initial Response
The simulation began with the “discovery” of a novel bacterium with high transmission rates. Participating countries were required to trigger their national alert frameworks. This phase prioritized the speed of information flow—testing how quickly data from a local health clinic could reach the WHO headquarters and, subsequently, other member states. Countries practiced "surge capacity" protocols, identifying which medical professionals could be mobilized to assist neighboring jurisdictions or partner nations.
Day Two: Sustained Management and International Coordination
The second day focused on the "stress test" phase. As the fictional outbreak intensified, the exercise introduced logistical bottlenecks and resource shortages. The 25+ partner organizations—ranging from the Africa Centres for Disease Control and Prevention (Africa CDC) to Médecins Sans Frontières—were brought into the fold. This phase was specifically designed to evaluate the "handshake" between global agencies and national governments, ensuring that technical expertise was delivered where it was needed most, without bureaucratic friction.
Supporting Data and Collaborative Networks
The success of Polaris II was marked by the diversity of its participants. The list of countries involved spanned all WHO regions, including Bangladesh, Brazil, Egypt, France, India, Kenya, Malaysia, and Yemen, among others. This geographical breadth is essential for a global response, as it accounts for varying levels of economic development and healthcare infrastructure.
Furthermore, the simulation served as a live-fire test for new collaborative bodies, most notably the Health Emergency Leaders Network for Africa and the Eastern Mediterranean. This network represents a strategic shift toward regionalized preparedness, allowing nations with similar geographic and socio-economic challenges to harmonize their responses before an crisis reaches the global stage.
The exercise also incorporated the expertise of seasoned emergency networks, such as:
- GOARN (Global Outbreak Alert and Response Network): Providing technical support for field operations.
- Emergency Medical Teams (EMT) Initiative: Coordinating the deployment of clinical personnel.
- Standby Partners: Facilitating the rapid logistics of non-medical support.
Official Responses: From Policy to Performance
The leadership at the WHO was unequivocal regarding the stakes of the exercise. Dr. Tedros Adhanom Ghebreyesus, WHO Director-General, framed the event as a testament to the necessity of the GHEC. “Exercise Polaris II showed what is possible when we act together. It demonstrated that global cooperation is not optional—it is essential,” he stated.
Dr. Tedros emphasized that the goal of the GHEC is to move beyond disparate national responses. "This is the purpose of the Global Health Emergency Corps: coordination across the emergency workforce, building trust, strengthening connections, and working as one across borders."
From the perspective of national implementation, the feedback was equally focused on practical utility. Edenilo Baltazar Barreira Filho, Director of the Public Health Emergencies Department at Brazil’s Ministry of Health, noted the shift from theory to reality. "By simulating the spread of a dangerous pathogen under real-life conditions, Exercise Polaris II helped us turn existing plans into action. It is not enough to have plans on paper—what matters is how they perform in practice."
Dr. Chikwe Ihekweazu, Executive Director of WHO’s Health Emergencies Programme, summarized the operational philosophy behind the exercise: “This reflects the spirit of the Global Health Emergency Corps: a well-organized, trained, coordinated and connected emergency workforce ready to respond wherever and whenever it is needed.”
Implications for Global Health Security
The implications of Polaris II extend far beyond the two days of the simulation. As part of the “HorizonX” program—WHO’s multi-year initiative for continuous simulation—Polaris II serves as a permanent fixture in the global health calendar.
1. Moving Beyond "Periodic Efforts"
Historically, pandemic preparedness has suffered from a "cycle of panic and neglect." Governments often invest heavily during a crisis, only to allow systems to atrophy once the threat recedes. HorizonX is designed to break this cycle by mandating that readiness remains a continuous, funded, and practiced investment.
2. The Role of Technology
The inclusion of AI-enabled planning tools in Polaris II indicates that the future of pandemic response will be data-driven. By automating the allocation of human resources and predicting potential hotspots, AI allows health ministers to make decisions based on real-time modeling rather than reactive intuition.
3. Equity as a Functional Strategy
The GHEC framework’s focus on equity is not merely a moral stance; it is a strategic one. The simulation highlighted that if a country cannot respond to an outbreak because it lacks the necessary workforce or resources, that outbreak will inevitably cross borders, affecting the entire world. Therefore, strengthening the capacity of the most vulnerable nations is the most effective way to secure the health of the most affluent.
Conclusion: A New Standard for Global Preparedness
As the world looks toward the future, the lessons learned from Exercise Polaris II provide a roadmap for resilience. The simulation did more than just test lines of communication; it built a human network of professionals who have now practiced the uncomfortable, high-stakes decisions required during a pandemic.
The World Health Organization’s theme for 2026, “Together for Health. Stand with Science,” is perfectly encapsulated by these exercises. By subjecting theoretical frameworks to the harsh realities of simulation, the global health community is ensuring that when the next real-world pathogen emerges, the response will not be defined by chaos, but by the coordinated, science-led, and unified action of a world prepared to stand as one.
Note: All references to Kosovo in the context of this exercise are made in accordance with United Nations Security Council resolution 1244 (1999).