In a monumental achievement for global public health, the World Health Organization (WHO) has officially validated Australia for the elimination of trachoma as a public health problem. This milestone marks the end of a decades-long battle against the world’s leading infectious cause of blindness, signaling a transformative victory for Indigenous Australians and providing a blueprint for the eradication of Neglected Tropical Diseases (NTDs) worldwide.
Australia now joins an elite list of 63 nations globally—and the 16th in the WHO Western Pacific Region—to have successfully eradicated at least one NTD. As the international community strives to meet the ambitious targets set out in the WHO road map for NTDs 2021–2030, Australia’s success offers both hope and a technical roadmap for other nations struggling with similar health inequities.
The Nature of the Threat: Understanding Trachoma
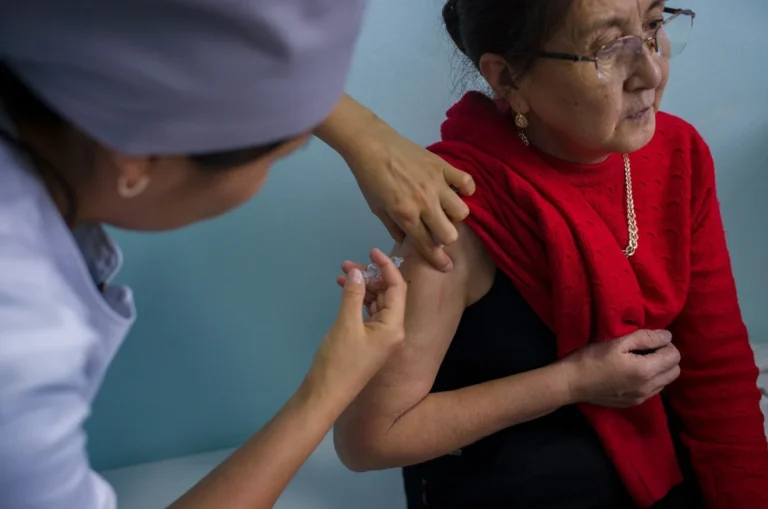
Trachoma is a devastating condition caused by the bacterium Chlamydia trachomatis. It is highly contagious, spreading through direct contact with infected individuals, contaminated clothing, and eye-seeking flies. While initial infections cause painful conjunctivitis, the true danger lies in its chronic nature.
Repeated infections over many years cause the inside of the eyelid to scar, eventually pulling the eyelashes inward—a condition known as trachomatous trichiasis (TT). When the eyelashes rub against the eyeball, it causes agonizing pain and permanent corneal scarring, which leads to irreversible blindness. Because it thrives in environments with limited access to clean water, sanitation, and hygiene, it has historically disproportionately affected the world’s most impoverished and marginalized populations.
A Chronology of Commitment: The Path to Elimination
Australia’s journey to this moment was not achieved overnight. While the disease had been largely eradicated from the majority of the Australian population in the 20th century, it persisted as a stubborn, hidden crisis within remote Aboriginal and Torres Strait Islander communities.
The Turning Point: 2006 and the SAFE Strategy
The pivotal moment in the nation’s fight came in 2006 with the launch of the National Trachoma Management Programme. This initiative was grounded in the WHO-recommended "SAFE" strategy, a comprehensive framework designed to break the cycle of transmission:
- S – Surgery: Providing corrective procedures for those already suffering from trichiasis to prevent further damage to their vision.
- A – Antibiotics: Implementing targeted, evidence-based treatment regimens to clear the infection within populations.
- F – Facial Cleanliness: Promoting health education and hygiene practices to reduce the spread of the bacteria.
- E – Environmental Improvement: Investing in the fundamental infrastructure of remote communities, including water access, sanitation, and housing, to eliminate the environments where the Chlamydia trachomatis bacterium thrives.
Sustained Action and Community-Led Success
The program was not merely a top-down government mandate; it was a collaborative, bottom-up effort. Coordination between federal and state governments, Aboriginal community-controlled health services, and local communities ensured that interventions were culturally safe and contextually relevant.
Unlike many international efforts that rely on mass drug administration, Australia utilized granular, community-level data to target interventions exactly where they were needed most. This nuanced approach, combined with long-term infrastructure improvements in remote areas, allowed the nation to see a steady, measurable decline in trachoma prevalence, eventually leading to the eradication of the disease as a public health concern.
Supporting Data and Technical Validation
The WHO’s validation process is rigorous and relies on stringent epidemiological criteria. To be declared free of trachoma as a public health problem, a country must meet specific thresholds:
- Trachomatous Trichiasis (TT): The prevalence of the blinding stage of the disease among those aged 15 and older must be less than 0.2%—a status defined as being "unknown to the health system."
- Follicular Trachoma (TF): The prevalence of the active infection in children aged 1–9 years must be less than 5% in each formerly endemic district.
- Surveillance: The existence of a robust, ongoing system to identify and manage any new incident cases of TT, ensuring that the disease does not re-emerge unnoticed.
Australia’s achievement of these benchmarks is a testament to the effectiveness of its integrated health surveillance systems. By weaving trachoma monitoring into the fabric of national health programs, Australia has ensured that its victory is not merely a snapshot in time, but a sustainable reality.
Official Responses and Reflections
The global health community has hailed the news as a triumph of persistence and partnership.
Dr. Tedros Adhanom Ghebreyesus, WHO Director-General, praised the nation’s dedication: “WHO congratulates Australia on this important achievement. This success reflects sustained commitment, strong partnerships, and a focus on reaching populations most affected by health inequities. It brings us closer to a world free from the suffering caused by trachoma.”
Domestically, the response has emphasized the role of First Nations leadership. Mark Butler, Minister for Health and Aged Care, noted that the success was a direct result of "Aboriginal and Torres Strait Islander leadership, community commitment, and sustained investment over many decades." He emphasized that the lessons learned during this campaign—particularly regarding community-led solutions—would serve as a model for addressing other preventable health conditions in remote and regional areas.
Malarndirri McCarthy, Minister for Indigenous Australians, echoed these sentiments, highlighting the central role of Aboriginal Community Controlled Health Organisations (ACCHOs). "This recognition reflects decades of work led by ACCHOs, alongside local health workers in remote First Nations communities. Their work has been critical to eliminating trachoma as a public health problem in Australia," she stated.
Dr. Saia Ma’u Piukala, WHO Regional Director for the Western Pacific, added a personal perspective: “As a doctor from Tonga, I’ve experienced these challenges for myself. But I also know that with strategic commitment underpinned by optimal resources and partnerships in health, success is possible.”
Broader Implications: Addressing NTDs Globally
The elimination of trachoma is not just a localized success; it is a significant contribution to the global effort to eradicate the 21 diseases categorized by the WHO as Neglected Tropical Diseases. These diseases affect more than 1 billion people worldwide, predominantly in underserved communities.
A Blueprint for the Future
Australia’s success demonstrates that even in geographically challenging, vast, and remote regions, the elimination of an NTD is possible when there is sustained political will and cross-sectoral collaboration. It underscores the necessity of addressing the "underlying determinants of health"—housing, water, and sanitation—rather than focusing on clinical treatment alone.
Furthermore, this achievement provides a roadmap for Australia itself. While the country has now eliminated trachoma, it continues to battle other endemic NTDs, such as Buruli ulcer, leprosy, and scabies. The mechanisms established through the trachoma program—particularly the integration of surveillance into standard national health systems—provide a scalable framework for tackling these remaining challenges.
Global Context and The Road to 2030
The 2021–2030 WHO road map for NTDs places a heavy emphasis on integration and country ownership. Australia’s validation as a trachoma-free nation provides an empirical success story that encourages other member states in the Western Pacific and beyond.
As the world looks toward the 2030 target, the focus remains on ensuring that progress is equitable. The WHO remains committed to supporting endemic countries, ensuring that surveillance is robust and that the gains made are protected by integrating NTD programs into the broader health sector.
Conclusion: A Legacy of Health
The elimination of trachoma in Australia is more than a medical milestone; it is a profound demonstration of what can be achieved when national policy aligns with the lived experiences and expertise of local communities. By placing Indigenous leadership at the center of the strategy, Australia has proven that health inequities are not insurmountable.
As we celebrate this achievement, the focus now shifts to maintenance and vigilance. The structures built to eliminate the disease will now serve as sentinels, ensuring that the health of all Australians—no matter how remote their home—remains a top priority. In the global fight against NTDs, Australia has moved from a nation burdened by a preventable, blinding disease to a beacon of success, lighting the way for the rest of the world.