Gdańsk, Poland – A groundbreaking systematic review published in the journal Cancers is shedding new light on the potential of optical coherence tomography (OCT) to revolutionize the surgical treatment of keratinocyte carcinomas (KCs), the most common form of skin cancer globally. The research, conducted by a team of dedicated scientists and medical professionals, suggests that this non-invasive imaging technology could significantly improve surgical precision, leading to better patient outcomes and reduced healthcare costs.
Keratinocyte carcinomas, encompassing basal cell carcinomas (BCCs) and squamous cell carcinomas (SCCs), are primarily caused by prolonged exposure to ultraviolet (UV) radiation. While typically having low mortality rates, their significant morbidity and potential for disfigurement necessitate meticulous surgical removal. The critical challenge in these procedures lies in accurately identifying and excising all cancerous tissue while preserving as much healthy surrounding skin as possible. This delicate balance is crucial for both oncological safety and optimal aesthetic results.
The Challenge of Margin Assessment in Skin Cancer Surgery
Current surgical approaches for KCs range from conventional excision to the more specialized Mohs micrographic surgery (MMS). Conventional surgery, while effective, often requires wider margins to ensure complete tumor removal, potentially leading to larger defects and the need for complex reconstructive procedures. MMS, considered the gold standard for high-risk KCs, offers superior margin control through immediate intraoperative histopathological examination of excised tissue. However, MMS is resource-intensive, time-consuming, and not widely accessible in many regions, creating a demand for alternative or adjunctive technologies that can enhance precision without the same logistical hurdles.

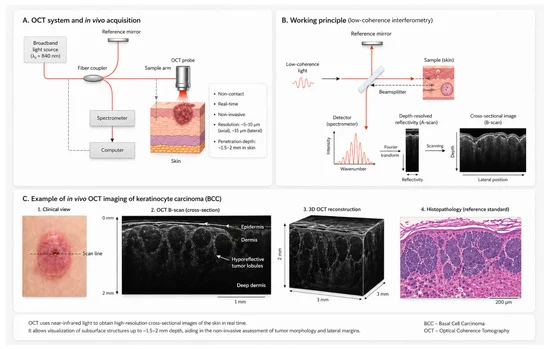
This is where optical coherence tomography enters the arena. OCT is a non-invasive imaging technique that uses light waves to capture real-time, high-resolution cross-sectional images of biological tissues. Its ability to visualize skin structures at a microscopic level, with resolutions typically between 5-10 micrometers, offers a promising avenue for real-time margin assessment during surgical procedures.
Groundbreaking Research Unveils OCT’s Potential
The systematic review, meticulously compiled by researchers Dana Bunevich, Monika Wojarska, Klaudia Kokot, and their colleagues, analyzed 11 studies involving a total of 303 patients. The objective was to evaluate whether in vivo OCT could serve as an effective adjunctive tool for delineating surgical margins in keratinocyte carcinomas.
The findings of this comprehensive review are highly encouraging. Across the included studies, a notable agreement between OCT imaging and traditional histopathology was observed, with agreement rates ranging from an impressive 84% to as high as 95.5%. This high concordance suggests that OCT can reliably identify cancerous tissue at the surgical margins.

Tangible Surgical Benefits Identified
Beyond diagnostic accuracy, the review highlighted direct surgical benefits associated with the use of OCT. In procedures utilizing Mohs micrographic surgery, the incorporation of OCT was associated with a significant reduction in the average number of MMS stages required. One study, for instance, demonstrated a decrease from an average of 1.89 stages to 1.23 stages, indicating fewer tissue layers needed to be removed to achieve clear margins. This translates to less tissue excision, shorter procedure times, and potentially reduced patient discomfort and recovery periods.
Furthermore, OCT-guided assessment was linked to narrower excision margins compared to those determined by clinical assessment alone. In some instances, OCT-identified margins were found to be narrower by an average of 0.4 mm, while still ensuring complete tumor removal. This precision minimizes the removal of healthy tissue, which is particularly valuable in cosmetically sensitive areas.
A Closer Look at the Technology and Its Application
The reviewed studies employed various OCT modalities, with conventional OCT being the most prevalent. Line-field confocal OCT (LC-OCT), a more advanced form, also showed promising results in one study, offering high resolution and a reasonable penetration depth. The application of OCT varied, with most studies focusing on its preoperative use for planning, while some explored its intraoperative utility to guide real-time excision.

The research also delved into the specific types of cancers and surgical techniques where OCT proved most beneficial. While the majority of studies focused on basal cell carcinomas (BCCs), a significant proportion also included squamous cell carcinomas (SCCs). Both conventional surgical excision and Mohs micrographic surgery benefited from OCT’s insights, underscoring its versatility.
Challenges and Future Directions
Despite the promising findings, the review also underscores the limitations that currently hinder the widespread adoption of OCT in clinical practice. The heterogeneity in OCT protocols, devices, and patient populations across the studies presents a challenge for drawing definitive, generalized conclusions. Moreover, the limited number of large-scale, randomized multicenter trials and the variability in lesion types and anatomical locations mean that further robust research is essential.
The depth of penetration of OCT, while superior to some other non-invasive imaging techniques, can still be a limitation for deeply infiltrative tumors. Additionally, the interpretation of OCT images requires specialized training and expertise, and potential imaging artifacts can occasionally lead to false-positive results, necessitating careful correlation with histopathology.

Looking ahead, the researchers emphasize the need for more extensive clinical trials. These trials should focus on standardized protocols, larger patient cohorts, and include cost-effectiveness analyses. Such studies will be crucial to validate the benefits of OCT, refine its application, and ultimately pave the way for its integration into routine dermatological and surgical practice.
Official Responses and Implications for Patient Care
While no direct official responses from regulatory bodies or major medical associations were included in the provided text, the publication of this systematic review in a reputable scientific journal like Cancers signifies a growing recognition of OCT’s potential within the medical community. The implications for patient care are substantial:
- Improved Oncological Outcomes: By providing real-time margin assessment, OCT can help ensure complete tumor removal, reducing the risk of recurrence.
- Enhanced Aesthetic Results: Minimizing the excision of healthy tissue leads to smaller defects, requiring less extensive reconstructive surgery and preserving cosmetic integrity.
- Reduced Healthcare Burden: Shorter procedure times, fewer repeat surgeries, and potentially fewer hospitalizations can lead to significant cost savings for healthcare systems.
- Greater Accessibility to Advanced Care: As OCT technology becomes more refined and its benefits are further validated, it could offer a more accessible alternative or complement to highly specialized procedures like Mohs surgery.
The journey of optical coherence tomography from an advanced imaging technology to a standard tool in skin cancer surgery is well underway. This comprehensive systematic review provides a critical roadmap, highlighting both the remarkable progress made and the essential steps required to fully realize its transformative potential in the fight against keratinocyte carcinomas. The future of skin cancer surgery appears brighter, more precise, and less invasive, thanks to the illuminating insights offered by OCT.