For generations, breast cancer has been framed almost exclusively as a women’s health issue. While pink ribbons and awareness campaigns have undoubtedly saved millions of lives through early detection and screening, this narrow focus has inadvertently fostered a dangerous misconception: the belief that men are immune to the disease.
The reality is far more sobering. Breast cancer does not discriminate based on gender. According to projections for 2025, approximately 2,800 men in the United States will be diagnosed with the disease, and 510 will succumb to it. These are not merely statistics; they are fathers, husbands, brothers, and sons who often find themselves navigating a medical landscape designed entirely for women.
The Reality of the Diagnosis: Jake’s Story
Among those facing this reality is Jake, a husband, father, and grandfather who found his life irrevocably altered by a diagnosis of Stage 4 estrogen receptor-positive (ER+) invasive ductal carcinoma (IDC).
Jake’s journey began with a subtle, persistent sign that many men would likely overlook: a small lump in his armpit. Despite the discomfort, he admitted to brushing it off for months. "I fell into the trap of the common misconception that men don’t get breast cancer," Jake admits. "I thought it was impossible, so I ignored what my body was trying to tell me."
That period of hesitation proved costly. By the time he sought medical intervention, the cancer had metastasized from his breast tissue to his hip. What might have been a highly treatable early-stage diagnosis had transformed into a complex, Stage 4 metastatic condition.
"Getting to that diagnosis was a bit of a journey, partly because male breast cancer tends to get caught later than in women," he explains. "Because the index of suspicion is so low, both for patients and sometimes even for primary care providers, it often reaches a more advanced stage before we finally find it."
A Chronology of Care and Miscalculation
The path from discovery to treatment is rarely linear, especially for men. For Jake, the initial medical assessment was fraught with uncertainty. He was first misdiagnosed with Stage 2 breast cancer, a classification that offered a more optimistic prognosis involving a standard regimen of chemotherapy, surgery, and radiation within a single year.

However, the nature of metastatic breast cancer (MBC) is notoriously unpredictable. As doctors investigated further, they discovered the cancer had moved to his hip bone. The diagnosis was recalibrated to Stage 4. This shift moved Jake from the realm of "curative" treatment into the reality of "chronic" management.
For the past two years, Jake has lived in a state of constant vigilance. His life is now measured in scans, blood tests, and the strategic rotation of therapies designed to keep the cancer at bay. "Living with breast cancer means I’m constantly on my toes," he says. "But I have an incredible team by my side, and that makes all the difference."
The Psychological Burden: Isolation in a Gendered System
Beyond the physical toll of chemotherapy and the systemic impact of metastasis, Jake highlights a secondary, equally debilitating struggle: the lack of gender-inclusive support.
"When the diagnosis finally came, it hit me with a whole mix of emotions: pure shock, total disbelief, and honestly, a real feeling of emasculation," he recounts. This emotional weight was compounded by a healthcare and support infrastructure that seemed entirely exclusionary.
"It was tough, especially because almost all the information and support out there seemed to be made for women. Every brochure, every website, it all said ‘she.’ That just made the whole experience feel really isolating and pretty awkward."
For many men, this linguistic and cultural barrier acts as a deterrent to seeking support. When a patient walks into a support group or opens a pamphlet only to find no reflection of their own experience, they are more likely to withdraw. Jake’s experience underscores a systemic failure: by ignoring the male experience, we are leaving a vulnerable population to navigate a life-threatening illness in silence.
Data and Demographics: Why the Gender Gap Persists
The data surrounding male breast cancer reveals a stark reality. While the incidence rate in men is significantly lower than in women—accounting for less than 1% of all breast cancer diagnoses—the mortality rate is disproportionately high.

Key Clinical Factors:
- Late-Stage Presentation: Men are more likely to present with larger tumors and regional lymph node involvement at the time of diagnosis compared to women.
- Biological Differences: Because men have less breast tissue, the cancer can spread to the chest wall or skin more rapidly.
- The "Awareness Gap": The lack of routine screening guidelines for men, combined with a societal stigma that equates breasts with femininity, leads to significant delays in patients reporting symptoms.
The medical community is beginning to acknowledge that "breast cancer" is a misnomer in terms of gender exclusivity. It is a disease of breast tissue, and since men possess this tissue, they remain at risk throughout their lives.
The Pivot to Advocacy: Shifting the Narrative
Jake decided that his experience could not end in silence. He turned to social media—specifically Instagram and TikTok, under the handle @theguywithstage4breastcancer—to dismantle the stigmas surrounding his condition.
"We’ve got to normalize it, push for early detection, and keep the conversation going about treatment," he asserts. His advocacy is not just about his own survival; it is about education. He uses his platform to remind men that any change in the chest area—a lump, swelling, or skin dimpling—demands immediate medical attention.
His message to other men is urgent: "Don’t brush off a lump or any weird changes because you think, ‘Oh, that’s a woman’s disease.’ It’s not. It’s everyone’s disease, and ignoring it could cost you a lot."
Implications for Healthcare and Society
The implications of Jake’s journey are clear: healthcare providers must adopt a gender-neutral approach to breast cancer education. If a patient presents with a suspicious mass in the chest area, clinical suspicion must be high, regardless of the patient’s sex.
Furthermore, there is a critical need for:
- Inclusive Resources: Patient support materials must explicitly include men, replacing gendered language with inclusive terminology.
- Increased Clinical Research: More research is needed into why male breast cancer behaves differently and how current treatment protocols—often derived from female-focused trials—can be optimized for male patients.
- Community Normalization: By sharing stories like Jake’s, the medical community can reduce the "emasculation" factor, encouraging men to seek help without fear of social judgment.
A Legacy of Purpose
For Jake, the diagnosis has become a catalyst for a broader movement. He envisions a world where a man diagnosed with breast cancer does not feel like an outlier, but rather part of a supported community.
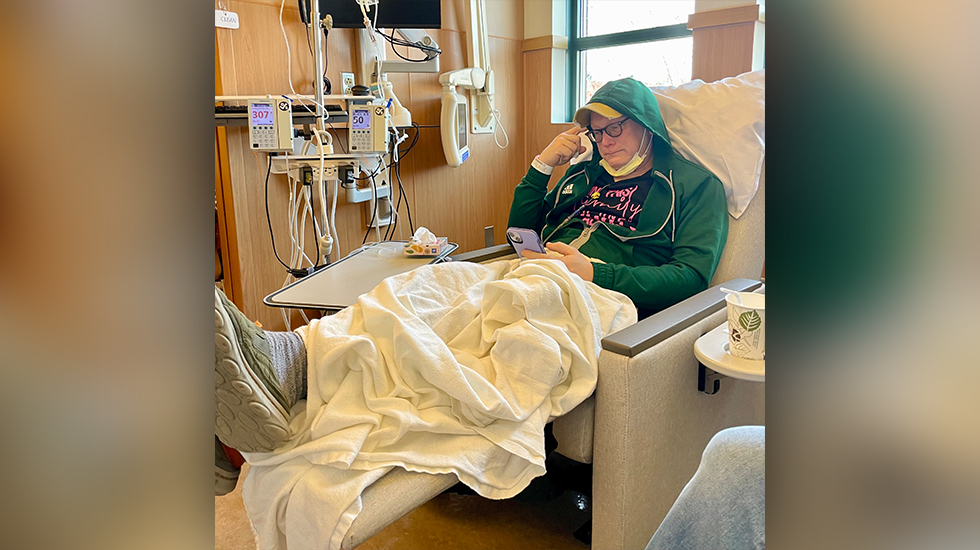
"My goal is to help build something bigger than my own story—a movement where every single person affected by breast cancer feels seen, supported, and gets the care they deserve," he says.
His advice to anyone—man or woman—facing a similar diagnosis is to become their own champion. "This fight is draining. Allow yourself to rest, to grieve, to connect with people who lift you up. Taking care of your mental and emotional health is just as critical as the physical treatments."
Resources for the Journey
For those seeking guidance, organizations like the National Breast Cancer Foundation (NBCF) offer specific support for patients navigating the complexities of a diagnosis. Whether it is connecting with a patient navigator, accessing educational guides on early detection, or joining support groups that welcome all, there are resources available to ensure no one has to face this journey alone.
As we look toward the future, the goal remains the same: to move past the outdated narrative that breast cancer is a gendered disease. By normalizing the conversation, we ensure that the next person who feels a suspicious lump—regardless of who they are—seeks the help they need early enough to change the outcome.
Jake’s story is a testament to the power of advocacy. By speaking out, he is not just fighting his own cancer; he is dismantling the barriers that have kept others in the shadows for far too long. In the face of a difficult diagnosis, he has chosen to turn his pain into purpose, reminding us all that the most powerful tool in medicine is awareness.