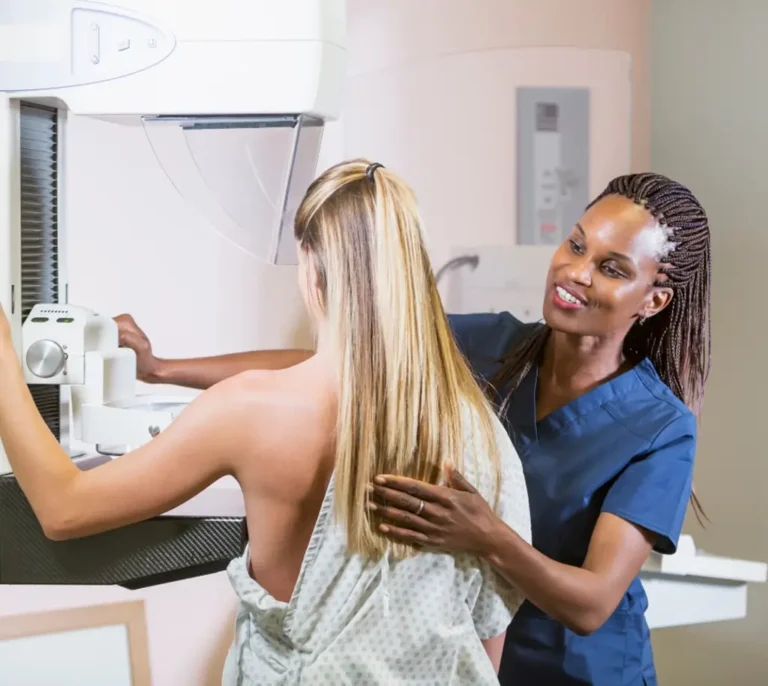
The journey through a cancer diagnosis is often described by patients not as a single event, but as an overwhelming odyssey through a complex and fragmented healthcare system. From the initial shock of biopsy results to the grueling cycles of chemotherapy, radiation, and long-term survivorship, the administrative and emotional burden can be as taxing as the disease itself. Recognizing the critical need for a more streamlined approach, Breast Cancer Canada (BCC) has announced the launch of a comprehensive national survey designed to evaluate the current state of cancer care navigation across the country.
This initiative seeks to capture a 360-degree view of the Canadian oncology landscape by gathering data from two primary stakeholders: the patients who rely on these services and the oncology nurse navigators who provide them. By identifying the disparities in care coordination, Breast Cancer Canada aims to provide a data-driven roadmap for systemic reform, ensuring that no patient is left to navigate the "cancer labyrinth" alone.
Main Facts: A Dual-Perspective Approach to Systemic Reform
The cornerstone of this initiative is its dual-perspective methodology. While many healthcare surveys focus exclusively on patient satisfaction, Breast Cancer Canada recognizes that the "view from the bedside" and the "view from the clinic" are equally vital to understanding systemic bottlenecks.
The Scope of the Survey
The survey is notably inclusive. Although spearheaded by Breast Cancer Canada, the organization has emphasized that the survey is open to all oncology patients and nurse navigators, regardless of the specific type of cancer. This broad scope acknowledges that while the biological treatments for breast, lung, or colorectal cancer differ, the logistical hurdles—such as scheduling multidisciplinary appointments, accessing financial aid, and managing transitions between hospital and home—are universal.
The Role of the Oncology Nurse Navigator
In the modern Canadian healthcare context, the oncology nurse navigator serves as the "glue" holding the patient’s experience together. These specialized professionals are responsible for:
- Clinical Guidance: Explaining complex diagnoses and treatment plans in plain language.
- Coordination: Managing the hand-off between surgeons, oncologists, and radiologists.
- Resource Connection: Linking patients to psychosocial support, nutritional counseling, and financial resources (often referred to as "financial toxicity" management).
- Advocacy: Ensuring the patient’s voice is heard during multidisciplinary tumor board meetings.
Key Objectives
The survey aims to pinpoint exactly where the Canadian system is succeeding and where it is failing. Specifically, it seeks to uncover:
- Consistency of Access: Why does a patient in an urban center have access to a dedicated navigator while a patient in a rural community might not?
- Breadth of Support: Are navigators empowered to provide emotional support, or are they restricted to purely administrative tasks?
- Continuity of Care: What happens to the patient once active treatment ends? Is there a "cliff" in support during the transition to survivorship?
Chronology: The Evolution of Cancer Care Navigation in Canada
To understand the urgency of this survey, one must look at the historical evolution of the Canadian oncology landscape.
The 1990s: The Birth of Navigation
The concept of patient navigation was pioneered by Dr. Harold P. Freeman in Harlem, New York, in 1990. His goal was to eliminate barriers to timely cancer care among underserved populations. By the late 1990s, Canadian provincial health authorities began to recognize that the increasing complexity of cancer treatments—shifting from simple surgeries to multi-modality therapies—required a dedicated coordinator.
2000–2015: Provincial Patchwork
During this period, various provinces began integrating "Patient Navigation" roles into their cancer agencies. However, because healthcare is provincially mandated in Canada, these roles developed in silos. In some provinces, navigation became a formal, nurse-led clinical role; in others, it remained a peer-support or volunteer-based model. This led to the "postcode lottery" of care, where the quality of support depended heavily on where a patient lived.
2020–2023: The Pandemic Catalyst
The COVID-19 pandemic exposed the fragility of these navigation systems. As surgeries were delayed and screenings were missed, the backlog of cases put immense pressure on nurse navigators. They became the primary point of contact for thousands of distressed patients. This period highlighted the necessity of a national standard for navigation, leading to the current initiative by Breast Cancer Canada.
2024: The Launch of the National Survey
In late 2024, Breast Cancer Canada officially opened the survey portals. The timing is strategic, coinciding with a national conversation about healthcare sustainability and the integration of digital health tools in oncology.
Supporting Data: The Rising Burden of Cancer in Canada
The necessity of this survey is underscored by sobering statistics regarding the prevalence of cancer and the current state of the nursing workforce.
The Growing Need
According to the Canadian Cancer Society, an estimated 2 in 5 Canadians will be diagnosed with cancer in their lifetime. With an aging population, the number of new cancer cases is expected to rise by approximately 40% by 2030. This surge will place an unprecedented load on the oncology infrastructure.
The Impact of Navigation on Outcomes
Peer-reviewed studies have consistently shown that effective navigation leads to:
- Reduced Emergency Room Visits: Patients with navigators are less likely to visit the ER for side-effect management because they have a direct line to a nurse who can provide early intervention.
- Improved Adherence: Patients are more likely to complete their full course of chemotherapy or radiation when they have a navigator helping them overcome logistical barriers like transportation or childcare.
- Reduced Time to Treatment: Navigation can shorten the window between a suspicious finding and the start of treatment, which is critical for aggressive cancers.
The Nursing Crisis
The survey comes at a time when Canada is facing a severe nursing shortage. A 2022 report by the Canadian Nurses Association suggested that Canada could be short nearly 117,000 nurses by 2030. Understanding the specific challenges of nurse navigators—who often face high rates of secondary traumatic stress and administrative burnout—is essential for retention and recruitment within the oncology sector.
Official Responses: Breast Cancer Canada’s Mission
While Breast Cancer Canada is primarily known for its commitment to funding life-saving research, the organization has increasingly focused on "the whole patient."
In statements surrounding the launch, the organization emphasized that research is only effective if patients can actually access the treatments resulting from that research. If a breakthrough drug exists but a patient cannot navigate the insurance hurdles or the hospital scheduling system to receive it, the research has failed its ultimate purpose.
"Cancer care is a journey that no one should have to walk alone," a spokesperson for the initiative noted. "By gathering this data, we are giving a voice to the thousands of patients who have felt lost in the system and the dedicated nurses who are working tirelessly to guide them. This is about moving from a system-centered model to a patient-centered model."
The organization also clarified that the confidentiality of the survey is paramount. Responses from nurse navigators are intended to be "brutally honest" regarding system capacity issues, without fear of professional repercussions, to ensure the data reflects the true reality of the front lines.
Implications: A Blueprint for the Future of Oncology
The results of this survey, expected to be analyzed and released in the coming year, will have far-reaching implications for Canadian healthcare policy.
1. Standardizing the Role of the Navigator
One of the primary goals is to create a national framework for what an "Oncology Nurse Navigator" actually is. By defining the scope of practice, Breast Cancer Canada can lobby for standardized training and certification, ensuring that a patient in Prince Edward Island receives the same caliber of navigation as a patient in British Columbia.
2. Influencing Funding and Resource Allocation
Data from the survey will be used to advocate for increased provincial funding. If the data shows that navigators are spending 60% of their time on paperwork rather than patient care, it provides a powerful argument for the integration of administrative assistants or better digital scheduling tools.
3. Addressing "Financial Toxicity"
Cancer often brings a heavy financial burden. The survey will likely reveal how well navigators are currently able to connect patients with financial aid. This could lead to better partnerships between healthcare providers and NGOs to provide travel grants, drug coverage assistance, and lost-wage support.
4. Improving Health Equity
The survey will provide insights into how navigation serves (or fails to serve) marginalized communities, including Indigenous populations, newcomers to Canada, and those living in extreme poverty. Identifying these gaps is the first step toward creating more equitable pathways to care.
Conclusion: A Call to Action
The success of this initiative depends entirely on participation. Breast Cancer Canada is calling on all those touched by the oncology system to contribute their experiences.
- For Patients: Your experience—whether positive or negative—is the evidence needed to demand better care for the next person diagnosed.
- For Nurse Navigators: Your expertise is the only way to identify the systemic barriers that prevent you from providing the care you were trained to give.
As Canada stands at a crossroads in healthcare delivery, data-driven initiatives like this survey offer a glimmer of hope. By listening to those who live and work within the system every day, Breast Cancer Canada is not just asking questions; they are building the foundation for a more compassionate, efficient, and unified cancer care system.
How to Participate:
- Patients: Cancer Patient Experience Survey
- Oncology Nurse Navigators: Oncology Nurse Navigator Survey
Participation is voluntary, confidential, and open to all cancer types.